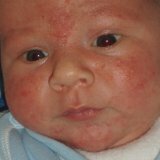
How to treat streptoderma in children?
Any skin purulent inflammatory diseases that are caused by streptococci in medicine are classified as streptodermia .To the disease began its development, you need only two factors - the presence of streptococci and damage to skin areas in which there is a decrease in protective function.Most often, the disease is diagnosed in childhood - this is associated with frequent skin lesions at this age, and the inability to constantly monitor compliance with personal hygiene.
Table of contents: Streptococcus How does streptodermia begin in children?What is the long-term course of streptodermia? The forms and symptoms of streptodermiaStreptococci
We recommend that you read:This is a conditionally pathogenic microorganism with which a person is constantly in contact - they "live" in the human gastrointestinal tract, both on the skin and in the respiratoryWays, and on all mucous membranes.Each person periodically becomes a carrier of streptococci, there are people who belong to the group of permanent carriers of these pathogenic microorganisms.But it is interesting that Staphylococcus always joins streptococci, which is the causative agent of streptoderma.
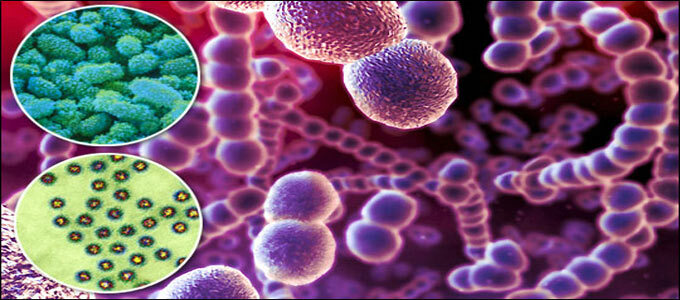
Streptococci have an amazing "survivability" - they instantly die only when boiled, but at a temperature of 60 degrees, the streptococcus continues to live for another 30 minutes; in chemical agents, these microorganisms die only after 15 minutes.
The considered pathogenic microorganism can cause a person to develop not only streptodermia, but also angina, bronchitis, myocarditis, erysipelas, meningitis, scarlet fever, glomerulonephritis and other diseases.
How does streptodermia start in children?
If the skin performs its protective functions for 100%, then streptococci do not generally cause a person any problems.But even a small damage to the skin disrupts the protective functions, the wound becomes the "gate" for infection - streptoderma develops.As a rule, the disease under consideration starts its development in places of scratches and rashes, insect bites( they are combed), cuts and abrasions.Even if streptodermia occurs without visible damage to the skin, it means that the injuries are simply invisible to the eye - they are microscopic, but sufficient for infection.
Once streptococci enter the damaged area of the skin, they begin to multiply actively and provoke the development of an inflammatory process that is not so easily treatable.
 Streptococcus can enter the area of damaged skin from a wide variety of locations:
Streptococcus can enter the area of damaged skin from a wide variety of locations:
- toys, utensils, towels and any household items;
- from a patient with streptodermia, sore throat, scarlet fever, pharyngitis;
- from the skin of the child;
- from the carrier, which is healthy and has no diseases.
If the development of streptoderma is associated with infection from an already sick person, then the course of the disease will be more rapid, aggressive and prolonged.Often streptoderma occurs as an epidemic - this usually happens in places of large concentrations of children( kindergartens, schools, community organizations).The incubation period of the disease in question is 2-10 days, it all depends on how strong the immune system is in a child.
In medicine, there are only three types of ways of infection with streptoderma:
- contact-household - toys, dishes, towels, bed-clothes, shoes, clothes;
- pin - hugs the sick child, kisses, close contact when playing;
- airborne - streptococcus falls on the skin of a child when sneezing or coughing is already a sick baby.
Note: airborne infection pathway is so rare that doctors do not usually notice it.
With what is the long-term course of streptodermia
In case of strong immunity and general health of the child, streptococci simply do not develop on the skin - the body copes with these pathogenic microorganisms on its own.But there are factors that contribute to the fact that the course of streptoderma will be prolonged, severe and with frequent relapses. Such provoking factors include:
- diagnosed helminthiases, anemia, hypotrophy, general intoxication of the body;
- chronic skin diseases - scabies, atopic dermatitis, pediculosis, allergic reactions;
- Rhinitis and otitis - discharge from the ears and nose act irritatingly on the skin;
- burns and / or frostbite;
- violation of personal hygiene rules, insufficient care for the child;
- long-term contact of damaged skin with water;
- no treatment for skin wounds.
Forms and symptoms of streptodermia
Doctors clearly distinguish symptoms with streptoderma - they are general in nature and inherent in all forms of the disease in question. Signs of streptodermia in childhood:
-
 body temperature rises to critical levels;
body temperature rises to critical levels; - headache and discomfort in the muscles and joints;
- nausea and vomiting;
- changes in the results of blood tests;
- violation of the general well-being of the child;
- in the area of foci of infection, there is an increase in lymph nodes.
The duration of the disease is too variable - from 3 to 14 days, it all depends on the individual characteristics of a particular child's body.
Doctors define several forms of the disease:
Impetigo streptococcal
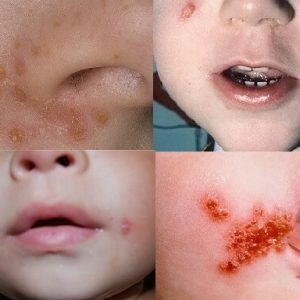
 This is the most common form of the disease, which is characterized by the appearance of specific eruptions on the face, hands, feet and other exposed areas of the body.Very often in childhood, is diagnosed with streptoderma of the nose - it also applies to the form in question.
This is the most common form of the disease, which is characterized by the appearance of specific eruptions on the face, hands, feet and other exposed areas of the body.Very often in childhood, is diagnosed with streptoderma of the nose - it also applies to the form in question.
Streptococcal impetigo is often found because in this case the infection does not penetrate deep layers of the skin, as its protective functions still persist, and local mechanisms of inhibition of the inflammatory process are included in childhood almost instantaneously.
Symptomatic of streptococcal impetigo:
- the skin does not change outwardly, it can only slightly blush.A bubble with a clear or turbid liquid inside, bordered by a reddish line appears on this place;
- , the liquid inside the bubble gradually becomes turbid, then it all bursts, and a light yellow crust forms in the place of the bubble;
- after the crust descends, there is a pink or cyanotic stain, which eventually disappears without a trace.
Please note: maturation period of each bubble is 5-7 days.
If streptococcal impetigo is noticed at the initial stage of development, then the treatment started can stop the development of the disease.But, as a rule, such a change in the skin is either simply not noticed, or not touched, in the hope that everything "will pass by itself".But the child begins to comb the formed crusts( itching is present during healing), from them follows a liquid, literally "stuffed" with streptococci.This liquid falls on healthy areas of the skin, remains on bed linens and clothes - the infection continues, the spread of the disease goes swiftly.
If the treatment and hygiene are not performed correctly, then streptococcal impetigo lasts for more than 4 weeks, and in some cases, the infection can even cause serious complications.
Bullous impetigo
This form of the disease is considered more severe and needs to be sought for professional medical care. Distinctive characteristics of the considered form of streptodermia:
-
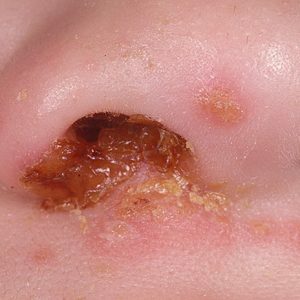
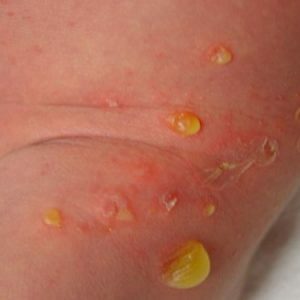 most often bullous impetigo occurs on the skin of the feet, shins and hands;
most often bullous impetigo occurs on the skin of the feet, shins and hands; - Bubbles larger than those with streptococcal impetigo are less strained, but the inflammatory process is more pronounced in them;
- to the main symptoms associated with high body temperature, changes in blood tests, enlarged lymph nodes;
- Bubbles in bullous impetigo are filled with serous fluid, burst extremely slowly and erosions form in their place.
Sleeve impetigo
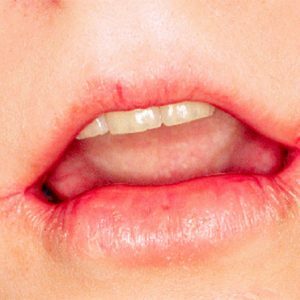 This is what people call - streptoderma appears in the corners of the mouth, it can rarely appear in the folds of the wings of the nose or the corners of the eyes.As a rule, the bubble appears single, even at dissection, the slick impetigo does not spread.
This is what people call - streptoderma appears in the corners of the mouth, it can rarely appear in the folds of the wings of the nose or the corners of the eyes.As a rule, the bubble appears single, even at dissection, the slick impetigo does not spread.
It is noteworthy that it is this form of the considered disease that is rapidly developing, does not show any additional symptoms and simply delivers some discomfort to the patient.Only in very rare cases, the slick impetigo passes into a chronic form of the flow with frequent relapses.
Erythemato-squamous streptodermia
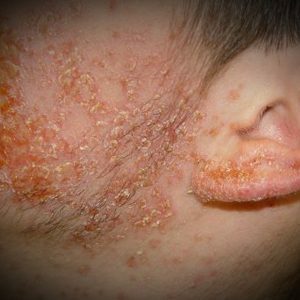
This is a dry appearance of the disease under consideration, which is most often present on the skin of the face - there are no damp blisters and red or bluish spots, only pink peeling spots are present in the lesions.
Erythemato-squamous streptoderma does not cause critical discomfort, is not prone to extensive spread, but is contagious - the treatment should be complete.
Surface Panicium
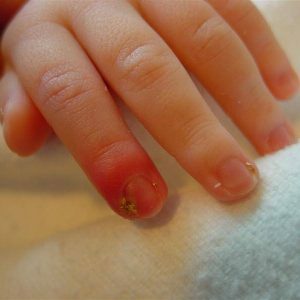 Panaritium occurs against the background of streptococcal impetigo, but only on the skin around the nail.The place of infection becomes inflamed, becomes red and swollen, characteristic bubbles appear, and then crusts.
Panaritium occurs against the background of streptococcal impetigo, but only on the skin around the nail.The place of infection becomes inflamed, becomes red and swollen, characteristic bubbles appear, and then crusts.
A prolonged course of superficial panarisation can lead to complete rejection of the nail plate.Doctors insist that this form of the disease requires intensive treatment.
Obstruction of streptococcal
 The peculiarity of this form of streptoderma is a secondary lesion against the background of classical diaper rash.Most often, streptococcal diaper rash appears in the behind-the-ear and underarms, folds and in the groin.
The peculiarity of this form of streptoderma is a secondary lesion against the background of classical diaper rash.Most often, streptococcal diaper rash appears in the behind-the-ear and underarms, folds and in the groin.
The considered form of streptoderma is difficult to treat, because when crusts appear on the skin, cracks appear, the streptococcal infection may join again.
Vulgar ecstema
This is a very severe form of streptoderma, characterized by the formation of ulcers and deep erosion. Distinctive characteristics of vulgar ecthyma:
-
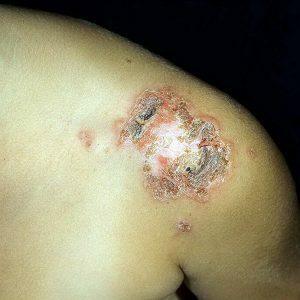
is formed on the buttocks, skin of the lower limbs, extremely rarely - on the hands and trunk;
- often occurs after previous viral diseases;
- can act as a complication of diabetes mellitus, hypovitaminosis, metabolic disorders;
- the course of the disease is always protracted, requires intensive treatment.
How is streptodermia diagnosed?
An experienced pediatrician or dermatologist will be able to diagnose the disease in question only by external signs.But often doctors make scrapings from affected areas of the skin - this will reveal the sensitivity of the pathogen to antibacterial drugs and quickly begin competent treatment.
In some cases, the specialist may prescribe an additional examination of the patient:
-
 feces analysis for egg worm;
feces analysis for egg worm; - urine analysis is common;
- blood test is biochemical and general;
- blood test for HIV infection.
How to treat streptodermia in children
Even if streptodermia occurs in a child in mild form, a full course of treatment is required.There are several activities that form a set of therapeutic measures.
Personal hygiene
Many parents are genuinely amazed that the child does not pass streptodermia even when using specific medications.This may be due to incorrect personal hygiene procedures.
Things to remember:
- For 3-4 days a child can not be bathed, even wetting with water, the affected skin areas are not necessary - water is an excellent conductor of infection.
-
 Unprotected skin areas should be wiped every day with a cotton swab dipped in ordinary warm water or in a decoction of chamomile and / or alternating stools.
Unprotected skin areas should be wiped every day with a cotton swab dipped in ordinary warm water or in a decoction of chamomile and / or alternating stools. - Always ensure that the child does not comb the lesion.In some cases, when intense itching is too troubling for the child, the doctor may prescribe antihistamines.
- A sick child should be given a separate towel, utensils, which must be carefully processed immediately after use.
- For the entire period of the disease, soft toys are removed from the child's field of vision, and plastic ones are washed daily and rinsed in boiling water.
- The child's bedding( especially pillow cases) must either be changed frequently, or ironed with a hot iron every day.
- If there are any small lesions on the skin, they should be wiped 2-3 times a day with any antiseptic solution.
Local treatment
Many recipes for the local treatment of streptoderma in children are already "ineffective" - many substances are simply discontinued, many are dispensed in pharmacies strictly according to prescription. But you can also use modern, very effective tools:
-
 salicylic alcohol;
salicylic alcohol; - hydrogen peroxide;
- fucorcin or boric acid;
- green.
It is necessary to apply antiseptics competently:
- first the vial is opened - extremely cautiously;
- then, with a cotton swab or cotton disc, apply an antiseptic to the area of the opened bubble and 1-2 mm around this place;
- it is necessary to wait until the antiseptic completely dries.
If we talk about folk remedies, the broths of chamomile medicinal, alternating and / or oak bark are approved even by official medicine - they are used as lotions and for washing the formed wounds.
Note: can not be folk remedies to treat streptoderma in a child - the skin is undergoing inflammation, there is a pathogenic microorganism, so you can not do without medications.
Antibiotics for streptodermia
Antibacterial drugs for streptodermia in children are taken orally and externally.But no doctor will appoint such aggressive medicines for single manifestations of streptoderma, mild form of the disease course.Antibiotics are prescribed only in extreme cases, when conventional means can not stop the process, and the child's condition worsens.
In some cases, doctors prescribe even drugs from the hormonal group, but this is an extreme measure.
For topical treatment, the following ointments with antibiotics are used:
-
 Tetracycline and erythromycin;
Tetracycline and erythromycin; - Mupirocin;
- Gentamicin and lincomycin;
- Levomekol;
- Baneocin;
- Bactroban;
- Altargo;
- Synthomycin.
Ointments with hormones, prescribed in extreme cases:
- Lorinden S;
- Canison plus;
- Belogent;
- Triderm;
- Betaderm and others.
If we talk about systemic treatment with antibiotics, then most often doctors use for this antibiotics penicillin group, cephalosporins or macrolides.Penicillins may not be prescribed if, in the recent past, the child has already received such treatment for any other disease, or there is an individual intolerance and hypersensitivity to such drugs.
Comparison of streptoderma with other diseases
Even experienced physicians admit that streptoderma is easily confused with some other skin diseases - at a certain stage of its development it simply takes other forms.But there are some differences - they will help you quickly find your bearings, make an accurate diagnosis and conduct effective treatment.
Pyoderma
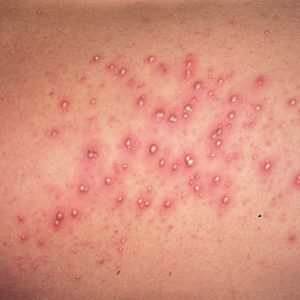 If to speak absolutely precisely, then streptoderma is one of the types of pyoderma - in medicine, all skin inflammatory pustular inflammations belong to the pyoderma group.But there is also a distinctive feature of this particular disease - the contents of streptodermial vesicles are never purulent, only serous.Even if there is some kind of pus in the liquid, it is minimal and does not make the contents cloudy.
If to speak absolutely precisely, then streptoderma is one of the types of pyoderma - in medicine, all skin inflammatory pustular inflammations belong to the pyoderma group.But there is also a distinctive feature of this particular disease - the contents of streptodermial vesicles are never purulent, only serous.Even if there is some kind of pus in the liquid, it is minimal and does not make the contents cloudy.
The greatest similarity is observed between pyoderma and vulgar impetigo - the symptoms are almost identical, even treatment will be identical.It is important at this point to pinpoint the type of pathogen and choose the right antibacterial agents for the course of treatment.
Herpes
The main difference between herpes and seizures is that in the disease under consideration the course of the disease is a swift, affected area falls precisely on the corner of the mouth, no spread to healthy tissues.
It is interesting that older children can pay attention to the itching, which appears on clean skin - it is a harbinger of herpes.But when zaedah itching appears only after the external manifestation of the disease.
Candidiasis of the corners of the mouth
In principle, this disease is easy to differentiate - cracks in the lesions are deep, there is a milky flight characteristic for thrush.
Varicella
Since the first rashes with this disease usually appear on the skin of the face and head, in the first hours you can take chickenpox for streptodermia.However, within a few hours other characteristic signs of chicken pox begin to appear - it is almost impossible to confuse it with streptodermia.
Allergic rash
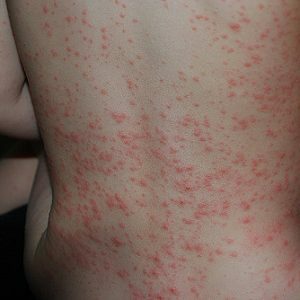 Even some experienced pediatricians can confuse the disease in question with a banal allergy.No, when the streptoderma vesicles are already fully formed and burst, it is not difficult to diagnose, but you can conduct a short test earlier: when you press on the allergic rash, the skin becomes white, with streptodermia, such changes in the color of the skin are not observed.
Even some experienced pediatricians can confuse the disease in question with a banal allergy.No, when the streptoderma vesicles are already fully formed and burst, it is not difficult to diagnose, but you can conduct a short test earlier: when you press on the allergic rash, the skin becomes white, with streptodermia, such changes in the color of the skin are not observed.
Note: syphilitic rash is also very similar to streptodermia, therefore, to differentiate the diagnosis, the doctor can refer the child for syphilis analysis.
Preventive measures
 Since the disease in question is contagious, the sick child is placed in quarantine for a period of 10 days.It is very important to introduce such a quarantine in a children's preschool, in a school or in mugs and sports palaces - in these very 10 days symptoms of streptodermia in other children may appear.
Since the disease in question is contagious, the sick child is placed in quarantine for a period of 10 days.It is very important to introduce such a quarantine in a children's preschool, in a school or in mugs and sports palaces - in these very 10 days symptoms of streptodermia in other children may appear.
As for the family, it is also necessary to carry out prophylaxis in case of an already sick child - everything comes down to observing the rules of personal hygiene.
If we talk about general prophylaxis, we can distinguish the reception of vitamin-mineral complexes, strict observance of the rules of personal hygiene and strengthening of immunity.
Streptodermia is an unpleasant disease that causes discomfort to the child.But there is a mass of modern medicines that greatly facilitate the condition of the child and promote a speedy recovery.
Tsygankova Yana Aleksandrovna, medical reviewer, therapist of the highest qualification category