Symptoms and treatment of peritonitis

Peritonitis is an inflammation of the peritoneum.The disease is considered within the concept of "acute abdomen", which is characterized by abdominal pain and muscle tension of the anterior abdominal wall.Despite the fact that every year the methods of treatment are improving more and more, peritonitis does not become less dangerous.The mortality rates for peritonitis are still quite high.So, with local peritonitis lethality is 4-6%, and with diffuse - more than 45%.
Table of contents: Causes of peritonitis Types of peritonitis SymptomsCauses of peritonitis
 Peritoneum is a serous membrane covering the abdominal cavity.The peritoneum, which lines the inner wall of the abdomen, is called parietal, and the surface of the organs is visceral.The total area of the peritoneum is approximately 2m2.
Peritoneum is a serous membrane covering the abdominal cavity.The peritoneum, which lines the inner wall of the abdomen, is called parietal, and the surface of the organs is visceral.The total area of the peritoneum is approximately 2m2.
Peritoneum has an absorption capacity, which is designated as a resorptive function.At the same time, it has the ability to release fluid, as well as fibrin into the abdominal cavity - this is an exudative function.Normally, these processes are balanced and in the abdominal cavity contains only a small amount of fluid between the peritoneal sheets.During the pathological state, the processes of exudation are activated, because of which a considerable volume of liquid can accumulate in the abdominal cavity.
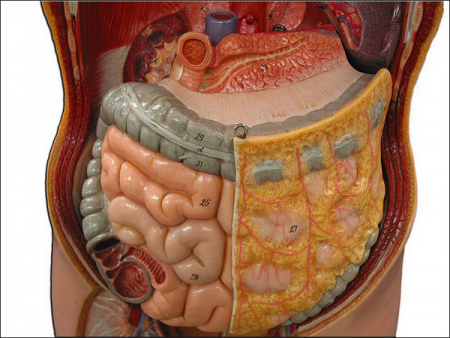
Peritonitis is primary when the disease develops due to ingestion of microorganisms into the abdominal cavity with blood or lymph flow, and secondary, when the disease develops in inflammation, perforation, damage to organs located in the abdominal cavity.
The following causes leading to the onset of peritonitis can be distinguished:
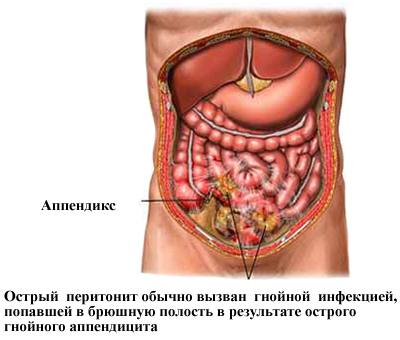
- Inflammatory processes occurring in the abdominal organs( appendicitis, cholecystitis, salpingitis, etc.);
- Perforation in the organs of the abdominal cavity( stomach or duodenum with ulcer disease, appendix with gangrenous or phlegmonous appendicitis, gallbladder with destructive cholecystitis, colon with ulcerative colitis);
- Damage to the abdominal organs;
- Operations performed on the organs of the abdominal cavity;
- Hematogenic peritonitis( pneumococcal, streptococcal, etc.);
- Inflammatory processes of any origin, not associated with abdominal organs( abdominal wall phlegmon, purulent processes localized in retroperitoneal tissue).
Distinguish between bacterial and aseptic peritonitis.The causative agents of bacterial peritonitis are both aerobic microorganisms( E. coli, Klebsiella, Proteus, Pseudomonas aeruginosa, Staphylococcus), and anaerobic( bacteroides, clostridia, peptococci).Often, peritonitis is provoked by a microbial association, that is, a combination of several microorganisms.
Aseptic peritonitis develops on contact of the peritoneum with blood, gastrointestinal contents, bile, pancreatic juice.It is noteworthy that after a few hours the microflora is involved in the pathological process and aseptic peritonitis becomes bacterial.
Types of peritonitis
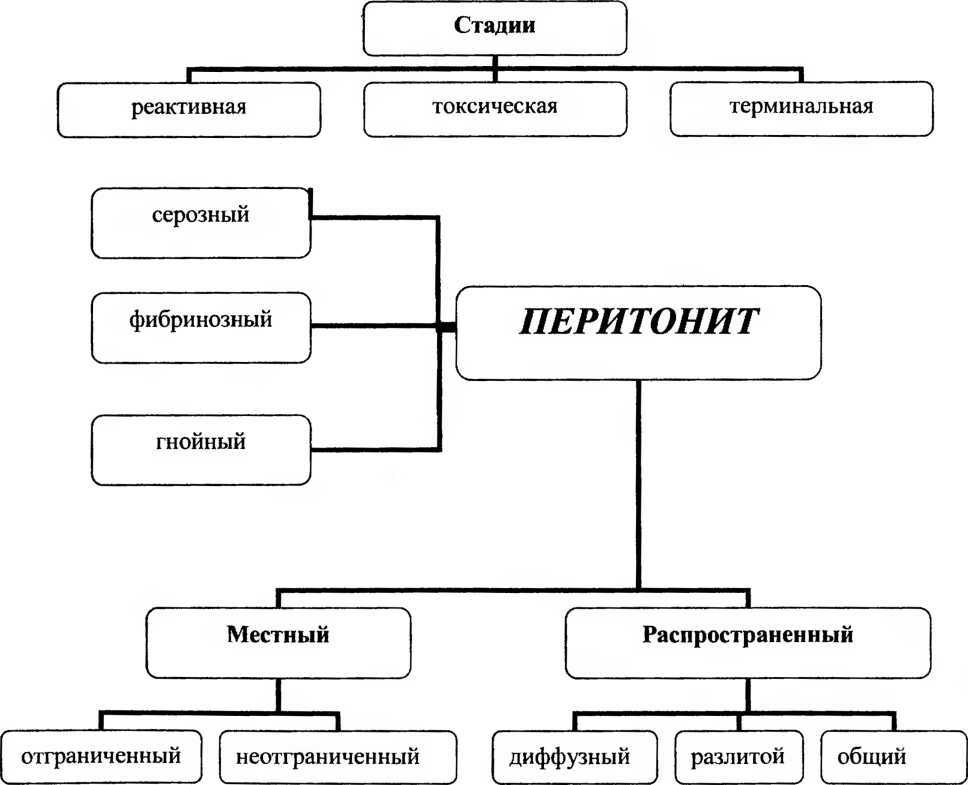
Depending on the prevalence of the inflammatory process, the following forms of peritonitis are distinguished:
- Local( occupies one anatomical abdominal cavity);
- Common( 2-5 anatomical abdominal parts are involved);
- Total( six or more anatomical areas of the abdominal cavity are involved).
It is also important to consider the type of exudate. So, depending on the nature of the exudate, these forms of peritonitis are distinguished:
- Serous;
- Fibrinous;
- Purulent;
- Hemorrhagic;
- Gallstick;
- Fecund;
- Mixed.
Peritonitis is also acute and chronic.Chronic form of the disease is more common in systemic infections of the body( syphilis, tuberculosis).Acute peritonitis occurs in three phases: reactive, toxic, terminal.
The first stage( reactive) is recorded in the first 12-24 hours of the disease.During this period, the peritoneum drains, exudates with the precipitation of fibrin.In the clinical picture, the local symptoms of the disease are especially pronounced.
The second stage( toxic) develops in 24-72 hours.During this period, toxicosis increases, resulting in general toxification symptoms prevail over the local.
The third stage( terminal) develops after 72 hours.This period is characterized by severe intoxication.
Symptoms of peritonitis
All symptoms observed in peritonitis can be divided into local and general.Local symptoms occur in response to irritation of the peritoneum with exudate, bile, gastric contents.These include abdominal pain, muscle tension of the anterior abdominal wall, as well as positive symptoms of irritation of the peritoneum, which can be revealed to the doctor when examined.Common symptoms develop against a background of intoxication of the body.These are nonspecific symptoms such as fever, weakness, tachycardia, nausea, vomiting, confusion.
In addition, the patient not only signs of inflammation of the peritoneum, but also symptoms of the underlying disease that provoked peritonitis.

Symptoms of the first stage of peritonitis
The first signs of peritonitis are a constant, not abating pain in the abdomen, which is amplified by changing the position of the body.Therefore, the patient lies on his back or on his side with the knees brought to his stomach and tries not to move again.The localization of pain depends on the location of the pathological process in the peritoneum.
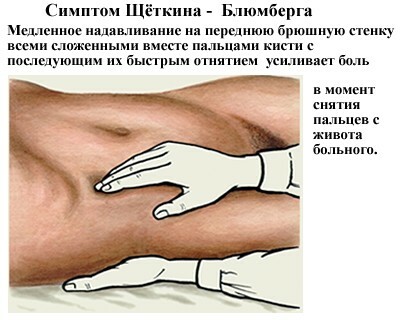
During the examination of the patient, the physician can detect the tension of the muscles of the anterior abdominal wall.With peritonitis, there are positive symptoms of irritation of the peritoneum.So, to determine the symptom of Shchetkin-Blumberg, you need to slowly press on the stomach, fix the hand for a couple of seconds, and then abruptly pull away.If at this moment there is a sharp pain, it means that a person has peritonitis.
The symptom of Mendel is determined by percussion( tapping) of the entire abdomen.According to the patient's reaction, the doctor can not only determine the intensification of pain, but also the localization of the pathological process.
Of the general symptoms, the patient has a fever, tachycardia, increased blood pressure, dry mucous membranes, and nausea with vomiting.
Symptoms of the second stage of peritonitis
 During this period, abdominal pain may become less pronounced.The tension of the muscles of the anterior abdominal wall, as well as the symptoms of irritation of the peritoneum, are present, but become less pronounced.At the forefront are such symptoms as stool retardation, flatulence, bloating caused by intestinal paresis.There is abundant vomiting with fetid odor.
During this period, abdominal pain may become less pronounced.The tension of the muscles of the anterior abdominal wall, as well as the symptoms of irritation of the peritoneum, are present, but become less pronounced.At the forefront are such symptoms as stool retardation, flatulence, bloating caused by intestinal paresis.There is abundant vomiting with fetid odor.
General toxification symptoms increase.The patient's heart rate increases( more than 120 beats per minute), blood pressure drops.The temperature rises, the tongue and mucous membranes of the mouth are dry, and the facial features are pointed.
Symptoms of the third stage of peritonitis
Intoxication becomes even more pronounced.Against the background of dehydration, the skin of the patient pales, facial features are sharpened, the mucous membrane of the mouth and the tongue are dry.Serious heart rate and low blood pressure are kept, and breathing becomes frequent, superficial.
The abdomen is swollen, the peristalsis is absent, there is abundant vomiting of gastric and intestinal contents.
Because of severe intoxication, the nervous system suffers: the patient is then adynamic, then falls into euphoria.There may be confusion, nonsense.
Diagnosis
For symptoms of an "acute abdomen", the following tests are performed:
- Clinical blood test - leukocytosis is noted, as well as a shift of the leukocyte formula to the left;Rectal and vaginal examination - allows to detect pronounced soreness of the rectum wall or vaginal vault caused by irritation of the pelvic peritoneum with peritoneal inflammatory exudate;
- X-ray examination of the abdominal cavity organs - allows to determine the blackout of the abdominal cavity due to the accumulated exudate in it;
- Ultrasound of the abdominal cavity - allows to detect the presence of free fluid.
- Laparocentesis( abdominal puncture) - allows you to examine the contents of the abdominal cavity;
- Laparoscopy - is conducted in case of doubt in the diagnosis.
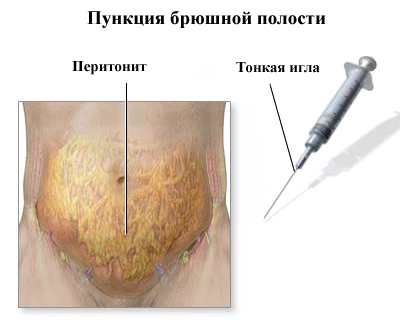
Treatment of peritonitis
Treatment of peritonitis is operative.The goal of surgical treatment is to eliminate the cause that led to the development of peritonitis, as well as drainage of the abdominal cavity.
The sequence of surgical procedures for peritonitis looks like this:
-
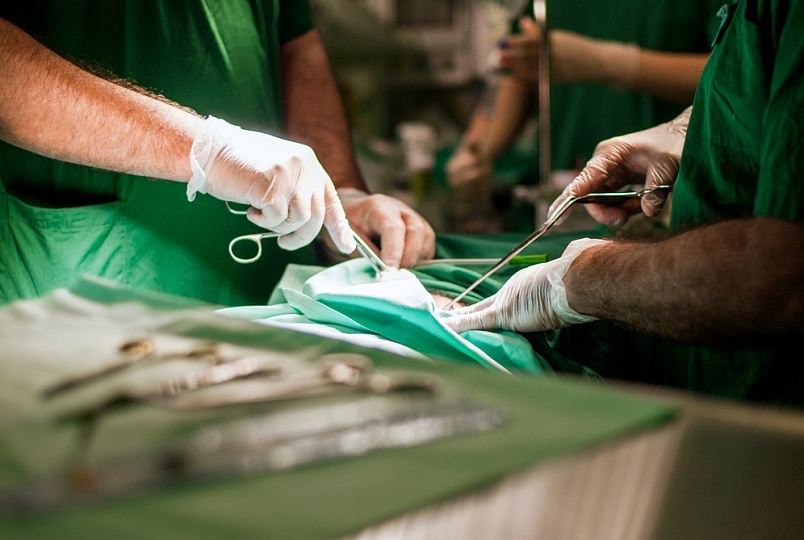 Preoperative preparation( gastrointestinal cleansing, anesthesia);
Preoperative preparation( gastrointestinal cleansing, anesthesia); - Laparotomy( cutting the anterior abdominal wall of the abdomen);
- Elimination of the source of peritonitis( removal of the appendix, gall bladder, resection of the ulcer, suturing the walls of the organ);
- Sanitation of the abdominal cavity( washing with antiseptic solutions);
- Decompression of the intestine;
- Introduction of drainage into the abdominal cavity;
- Wound closure.
The prognosis for recovery is better the earlier the operation was performed.Optimal operation in the first hours of the disease.Operative intervention, conducted a couple of days after the appearance of the first symptoms, significantly reduces the patient's chances of recovery.Therefore, when there is pain in the abdomen, you can not hesitate, you need to see a doctor immediately.
In addition, the treatment of peritonitis is supplemented with medication.The purpose of drug treatment is the elimination of pathogenic microflora, as well as the correction of metabolic disorders. The following groups of drugs are used:
- Antibiotics - use predominantly broad-spectrum antibiotics( gentamicin, sigmamicin, benzylpenicillin, ampicillin, ceftriaxone);
- Detoxifying agents( 10% calcium chloride solution);
- Infusion solutions( 5% and 25% glucose solutions, hemodez, solutions of Ringer, Hartmann);
- Colloidal preparations and protein preparations of blood( plasma, albumin, protein);
- Diuretics( furosemide, mannitol);
- NSAIDs( ibuprofen, paracetamol);
- Antiemetic drugs( metoclopramide);
- Anticholinesterase drugs( proserin) - are used to prevent the development of intestinal paresis.
Note: , if you have abdominal pain, do not prescribe yourself an analgesic medication.This will lead to the fact that the symptoms of the disease will become less pronounced and questionable, which will make it difficult for the doctor to determine the correct diagnosis.
Post-operative care
After the operation, it is important to continue drug treatment to prevent complications.
On the second day after the operation, parenteral nutrition begins.The volume of infusion therapy is approximately 50-60 ml per kilogram of body weight per day.When restoring intestinal motility enter enteral nutrition: the introduction of nutrient mixtures using a probe through the mouth and nose.The composition of the mixtures and the duration of such feeding is determined by the doctor.
 With positive dynamics, the restoration of the normal operation of the intestine goes to natural nutrition.This occurs usually no earlier than the fifth day after the operation.It is necessary to adhere to a low-calorie diet.In this period it is recommended to eat lean meat broths, vegetable purees, kissels and compotes.Gradually increase the caloric content of the diet, adding meat, eggs, dairy products to it.You can not eat rich meat broths, smoked products, spices, confectionery, chocolate, coffee, carbonated drinks, beans.
With positive dynamics, the restoration of the normal operation of the intestine goes to natural nutrition.This occurs usually no earlier than the fifth day after the operation.It is necessary to adhere to a low-calorie diet.In this period it is recommended to eat lean meat broths, vegetable purees, kissels and compotes.Gradually increase the caloric content of the diet, adding meat, eggs, dairy products to it.You can not eat rich meat broths, smoked products, spices, confectionery, chocolate, coffee, carbonated drinks, beans.
Several times a day you need to inspect the postoperative wound, pay attention to the purity of the dressing, the degree of blotting.The bandage should be changed regularly.When changing the dressing, you must follow the rules of antiseptic and do not allow the drainage tube to move.
Grigorova Valeria, medical reviewer