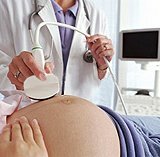
Obstetric peritonitis in the postpartum period
 Peritonitis inflames the peritoneal cavity. In addition to inflammation, the functions of certain body systems are disrupted, which leads to severe complications. Obstetric peritonitis is one of the most severe forms of postpartum infection, which can develop as a result of destruction of purulent structures in the appendages of the uterus, cholecystitis, appendicitis and pancreatitis. But most often the cause of obstetric peritonitis is complications after caesarean section.
Peritonitis inflames the peritoneal cavity. In addition to inflammation, the functions of certain body systems are disrupted, which leads to severe complications. Obstetric peritonitis is one of the most severe forms of postpartum infection, which can develop as a result of destruction of purulent structures in the appendages of the uterus, cholecystitis, appendicitis and pancreatitis. But most often the cause of obstetric peritonitis is complications after caesarean section.
Pseudo-inflammatory complications after caesarean section most often occur for the following reasons:
- Caesarean section is performed on the uterus, resulting in impaired integrity of lymphatic and blood vessels. This promotes direct bacterial invasion of the lymphatic and circulatory system of the uterus;
- An operation that is performed against the background of chorionamnionitis causes a direct spread of the infection to the peritoneum, which leads to the onset of early peritonitis;
- Infectious agents that are in the area of the scar on the uterus, multiply rapidly and spread beyond the wound;
- Sutures on the uterus interfere with complete uterine contraction in the postpartum period, this disrupts the normal outflow of bloody discharge. As a result, favorable conditions are created for the reproduction of microorganisms.
Statistics suggest that obstetric peritonitis occurs in 30% of cases due to infection of the peritoneum during surgical intervention, which was performed against the backdrop of a latent chorioamnionitis. Consequently, in this case, the source of infection is the contents of the uterus, which fell during the opening of the uterus in the abdominal cavity. In 55% of cases, the disease develops due to the inferiority of the sutures on the uterus - after a while the seams diverge and secondary peritonitis occurs. In 15% of cases, peritonitis occurs as a result of a violation of the barrier function of the intestine - the infection penetrates through the walls of the intestine into the abdominal cavity. Very rarely, peritonitis occurs due to the rupture of purulent lesions in the uterus.
What triggers obstetric peritonitis in the postpartum period?
After cesarean section, the pathophysiological changes in peritonitis are determined not only by the type and quantity of microorganisms that have entered the abdominal cavity, but also by environmental factors, and by the rate of reproduction of microorganisms.
Not always to the development of peritonitis leads to a single infection of the abdominal cavity during surgery. A huge role is played by the general state of health of a pregnant woman, as well as the body's resistance to infections. In addition, it is necessary to take into account the factor that weakening of immunity after Caesarean section. The cause of this is increased blood loss, postoperative stress, violation of blood microcirculation and the like.
Obstetric peritonitis can result from a chronic foci of infection in the form of endometritis in the postpartum period or chorioamnionitis during labor. Chorioamnionitis can develop as a result of a prolonged anhydrous span. If you have it, you can not do caesarean section, but sometimes doctors do not take this factor into account.
Most often, peritonitis after caesarean section occurs in women with:
- , the duration of the birth process is more than 12 hours;
- exacerbation of chronic infections;
- anhydrous interval more than 6 hours.
After cesarean section, the species composition of the microflora of the genital tract changes significantly. Before the operation monocultures of conditionally pathogenic microflora prevail, and enterobacteria predominate after the operation. Their number increases significantly in the first days after the caesarean section. If the operation passes without complications, then the usual microflora of the genital tract gradually displaces microorganisms that are not common to the birth canal. With reduced immunity in the first three days after the operation, the opportunistic microflora is very strongly activated. As a result, microorganisms can enter the uterus and lead to the development of an inflammatory process.
What happens during obstetric peritonitis in the postpartum period?
The leading role in the pathogenesis of peritonitis is played by intoxication. Disease-causing bacteria actively release substances that accumulate in the tissues and lead to an inflammatory process. Toxic products are absorbed into the blood and carried throughout the body. Thus, they have a negative effect on the nervous apparatus of the intestine and the central nervous system. Exchange processes in all tissues of the body are violated, and this leads to disruption of the functions of the cardiovascular system, kidneys, liver and respiration.
If during the time you do not detect obstetric peritonitis and do not start treatment, the symptoms can be life-threatening: edema of the uterus, abdominal organs, lungs and even the brain develops. Due to impaired vascular permeability, absorption processes are disrupted, and a lot of fluid accumulates in the intestine. The patient may experience nausea and severe vomiting, and more often in inflammatory processes, the body temperature rises. Often this leads to multi-organ failure: pulmonary, cardiac, renal, hepatic, to the development of DIC syndrome.
A special place in the pathogenesis of peritonitis, which arose after cesarean section, takes paresis of the intestine. There is a hyperextension of the intestine loops with gases and liquid, as a result of which its functions( secretory, motor and absorbed) are disrupted and the body is dehydrated. Because of all the above symptoms, a woman with peritonitis feels a sharp pain in the abdomen.
Symptoms of obstetric peritonitis in the postpartum period
Because of the active multiplication of pathogens in the damaged cavity, pus begins to accumulate. In addition, very often physicians notice the allocation of a large number of blood supplements and blood. Obstetric peritonitis is characterized by three phases.
The first phase - the initial phase, lasts 24 hours. At this phase, the maximum severity of general clinical symptoms occurs: protective tension of abdominal muscles, abdominal pain, digestive disorders( diarrhea and vomiting), motor excitation, increased respiratory rate and pulse, increased blood pressure.
The second phase is toxic, lasting from 24 hours to 72 hours. During this period, hemodynamics, microcirculation of blood are disrupted, kidney and liver function is disrupted, hypoxia is increasing and tissue respiration worsens. Protective muscle tension and pain syndrome decrease against a background of severe oppression of the intestinal peristalsis, while the flatulence increases. A syndrome of multiple organ failure is formed.
The third phase is terminal, comes after 72 hours. At this phase, doctors observe a complete absence of intestinal peristalsis, strongly pronounced meteorism, painful sensations strong. The patient may experience painful shock.
The most effective treatment in the first phase. In the second and third phase, the prognosis for complete recovery is not very successful. However, the success of treatment depends on many factors: the variant of infection, the amount of blood loss during cesarean section, the functional disorders of the gastrointestinal tract, and the like.