Adrenalectomy
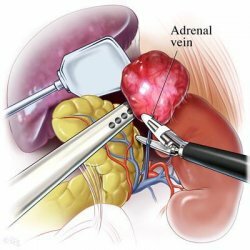 Adrenalectomy is a surgical operation for unilateral removal of the adrenal gland( adrenal gland).Usually conducted in connection with the development of adrenal tumor lesion. The operation can be performed both for the removal of one adrenal gland and for bilateral removal of the adrenal glands( bilateral adrenalectomy).In benign or inactive tumors of the adrenal gland, partial adrenalectomy is practiced, in which only the tumor( adenoma, cyst) is removed without removing the adrenal gland itself. The resulting biopsy is sent for histological analysis to obtain an opinion on the type and cause of the tumor. Such an organ-preserving operation makes sense if the patient has different adrenal glands and a chance to keep the adrenal gland, since when removing both adrenals, a person becomes dependent on hormone replacement therapy for life.
Adrenalectomy is a surgical operation for unilateral removal of the adrenal gland( adrenal gland).Usually conducted in connection with the development of adrenal tumor lesion. The operation can be performed both for the removal of one adrenal gland and for bilateral removal of the adrenal glands( bilateral adrenalectomy).In benign or inactive tumors of the adrenal gland, partial adrenalectomy is practiced, in which only the tumor( adenoma, cyst) is removed without removing the adrenal gland itself. The resulting biopsy is sent for histological analysis to obtain an opinion on the type and cause of the tumor. Such an organ-preserving operation makes sense if the patient has different adrenal glands and a chance to keep the adrenal gland, since when removing both adrenals, a person becomes dependent on hormone replacement therapy for life.
Morphology and location of the adrenal glands
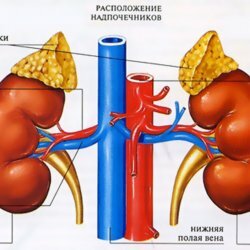 The adrenal glands are a paired organ located above the upper poles of the kidneys lateral to the spine. Each adrenal gland has an average weight of 4 grams. The right adrenal gland is in contact with the inferior vena cava and the liver. The left adrenal gland is attached to the pancreas and splenic vessels. Behind, both adrenal glands touch the diaphragm. The adrenal gland itself consists of two layers - cortical( external) and cerebral( internal).Both layers have a different embryonic origin and produce different hormones. The cortical layer is responsible for the production of corticosteroids and sex hormones, and cerebral for catecholamines( epinephrine, norepinephrine, dopamine) and some peptides. Together with the kidneys, the adrenal glands are encapsulated in a fat capsule and covered with a renal fascia.
The adrenal glands are a paired organ located above the upper poles of the kidneys lateral to the spine. Each adrenal gland has an average weight of 4 grams. The right adrenal gland is in contact with the inferior vena cava and the liver. The left adrenal gland is attached to the pancreas and splenic vessels. Behind, both adrenal glands touch the diaphragm. The adrenal gland itself consists of two layers - cortical( external) and cerebral( internal).Both layers have a different embryonic origin and produce different hormones. The cortical layer is responsible for the production of corticosteroids and sex hormones, and cerebral for catecholamines( epinephrine, norepinephrine, dopamine) and some peptides. Together with the kidneys, the adrenal glands are encapsulated in a fat capsule and covered with a renal fascia.
Indications for operation
- Adrenal cancer( cortical cancer).
- Diseases, adrenal gland disorders, in which too much of one hormone is produced( Cushing syndrome, pheochromocetoma, aldosteroma, carcinoma adenoma).
- Large mass of the adrenal gland.
- Adrenal disorder of an unclear etiology.
Diagnosis of adrenal tumors
The dimensions, location and presence of adrenal tumor metastases are well defined by ultrasound of the adrenal gland, computed tomography( CT) or magnetic resonance imaging( MRI).To determine the hormonal activity of the tumor, a blood and urine test is performed. In some cases, a biopsy of the affected area is made to confirm the diagnosis.
Methods of adrenalectomy
 Traditional adrenalectomy-cavitary laparotomy performed through an abdominal opening( transabdominal) or thoracic cavity( thoracoabdominal).It is used for the removal of extensive malignant tumors with the damage of closely located organs and tumors larger than 10-12 cm. After the seam remains about 20-30 cm.
Traditional adrenalectomy-cavitary laparotomy performed through an abdominal opening( transabdominal) or thoracic cavity( thoracoabdominal).It is used for the removal of extensive malignant tumors with the damage of closely located organs and tumors larger than 10-12 cm. After the seam remains about 20-30 cm.
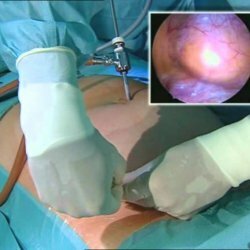
Laparoscopic adrenalectomy .Most often it is currently practiced in view of minimally invasive, it is considered a disadvantage to increase the duration of the operation( in comparison with the open operation, the time is increased by 20 minutes).Produced through 4 small incisions( about 1.27 in diameter) using a special endovideoscopic technique. There are two types of adrenal access during the operation:
Laparoscopic retroperitoneoscopic access .The operation is performed from the side of the back without entering the abdominal cavity. This type of adrenalectomy is the most effective and safe, because the risk of damage to the abdominal cavity is minimal. The patient is placed on the operating table lying on his stomach, a special gas acting as a contrast is inserted through the incision into the retroperitoneal space, thereby providing the surgical field to the surgeon. Further, depending on the type of retroperitoneoscopic adrenalectomy:
- with traditional retroperitoneoscopic adrenalectomy( CORA), the surgeon introduces 2-3 trocar for endoscopic instruments( video camera, scissors, clamps, coagulators, etc.).
- with a single-port retroperitoneoscopic adrenalectomy( SARA) through a single incision 3 cm long, an endoscope and one instrument are introduced. After the operation, there is practically an inconspicuous scar in the lumbar region.
Laparoscopic transabdominal access - is performed through the abdominal cavity using endosurgical instruments. There are two types:
- laparoscopic transabdominal lateral access. The patient is placed on his side( opposite to the affected adrenal gland), the surgical table is brought to a position of 30 degrees in the lumbar region, securely fixed. Further, gas is injected into the hypochondrium space and trocar for manipulators. Enter the abdominal cavity, remove the internal organs and after the passage of the posterior peritoneal wall proceed to remove the adrenal gland.
- laparoscopic transabdominal direct access. The patient lies on his back, also with the slope of the table in the lumbar region. This access is convenient in that it provides the surgeon with a larger working volume and access to both adrenal glands.
Contraindications to laparoscopic operation
Absolute:
- terminal states of the patient, coma;
- progressive decompensation of cardiopulmonary activity;
- sepsis, diffuse purulent peritonitis;
- other pathologies and conditions with a high risk of surgical intervention;
General:
- obesity in the last stage( more often referred to as relative contraindications);
- coagulation system;
- local or diffuse peritonitis or suspected of it;
- late pregnancy;
- common infectious diseases;
Local:
- infection in anterior abdominal wall;
- previously performed on the abdominal cavity open surgery, adhesions in the abdominal cavity, scar deformities of the abdominal wall;
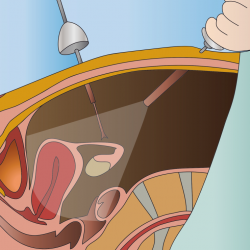 The decision in favor of an open surgery is influenced by such conditions of the patient as the presence of signs of adrenal cancer with growth in closely related tissues and organs( a wide revision of the retroperitoneal space is required) and a tumor more than 10cm( due to the complexity of its removal and an increase in the patient's time under general anesthesia with laparoscopicOperation).
The decision in favor of an open surgery is influenced by such conditions of the patient as the presence of signs of adrenal cancer with growth in closely related tissues and organs( a wide revision of the retroperitoneal space is required) and a tumor more than 10cm( due to the complexity of its removal and an increase in the patient's time under general anesthesia with laparoscopicOperation).
Preoperative preparation
On the eve of surgery, the patient is prohibited from eating food, this is associated with the risk of asphyxia vomit during anesthesia. Immediately before the operation, premedication is performed( drugs are introduced that facilitate and enhance the effect of anesthesia).In the operating room, a catheter is inserted into the ulnar vein to administer the drugs before and during surgery, anesthesia and anesthetics. A special respiratory mixture is passed through the mask and the patient is immersed in sleep( anesthesia).After intubation, the trachea starts adrenalectomy.
Possible complications in
- operation blood pressure lowering( when the central adrenal vein is compressed)
- bleeding
- damage to other organs
- adverse reaction to anesthesia
Postoperative period
Open surgery is a great stress for the body. In the first hours after the operation, narcosis gradually stops, strong painkillers are administered. Observe the drainage. Food intake during the first hours after surgery is prohibited, nutrients come parenterally with infusion therapy. Carefully observe the work of the gastrointestinal tract to exclude the development of adhesions. Postoperative sutures are processed daily. In laparoscopic surgery, bed rest is up to 1 day. If the puncture sites were sutured with absorbable suture material, no stitches are required, if non-absorbable threads - sutures are removed for 5-7 days, more often in the out-patient clinic. Primary nutritional restrictions are mostly related to anesthesia. With unilateral adrenalectomy, the entire load is transferred to the remaining adrenal gland( for the prevention of adrenal insufficiency, steroid hormones are administered), and with bilateral adrenal removal, hormone replacement therapy is prescribed.
Possible postoperative complications
- bleeding
- thromboembolic complications( phlebothrombosis, pulmonary embolism)
- postoperative intestinal paresis
- pulmonary complications(
- adrenal insufficiency( expressed as hypotension, hypoglycemia, hyponatremia, temperature, confusion,weakness)
- infectious purulent wound