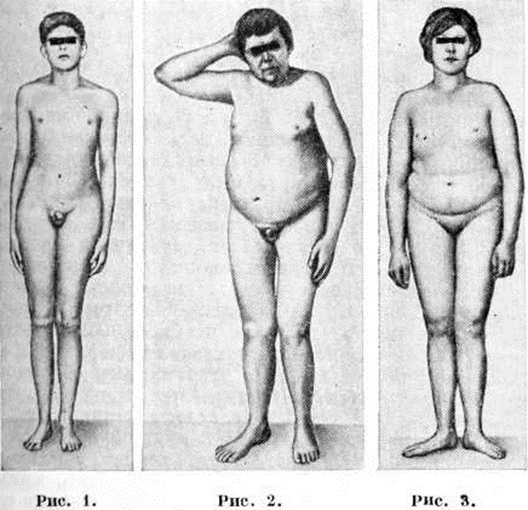
Insulinoma of the pancreas: symptoms, diagnosis and treatment
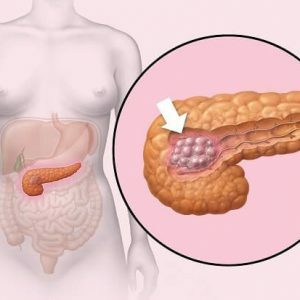
Insulinoma is a benign( less often malignant) pancreatic tumor that develops against the backdrop of pathological growth of β-cells located in the so-called."Islets of Langerhans."It is characterized by autonomous hormonal activity.With this pathology, the hormone insulin is produced in excess, which leads to severe hypoglycemia.
Note: for hypoglycemia is understood as a low level of glucose in the blood.
The tumor is able to develop in any part of the gland.Sometimes its extrapancreatic localization with its location in the liver, epiploon, gastric wall, etc. is revealed. Usually its dimensions do not exceed one and a half to two centimeters in diameter.
According to medical statistics, up to 15% of insulin is of a malignant nature.In every third case they give secondary foci - metastasis.
Table of Contents: 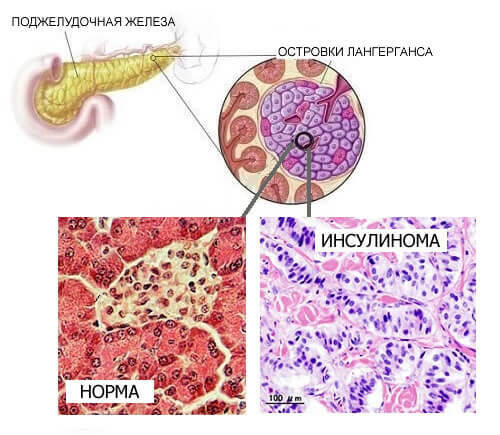
In patients with insulinoma, patients suffer from hyperinsulinism and accompanying hypoglycemic attacks of insulinoma.
In particularly severe situations, convulsions develop.The patient against a background of a sharp drop in blood glucose can fall into a coma.
Uncontrolled production of insulin often develops a hypoglycemic syndrome, which is a combination of a number of disorders of neuroglycopenic and adrenergic origin.
The cause of hypoglycemia is the completely autonomous insulin synthesis by β-cells and the release of this hormone responsible for the utilization of glucose into the systemic bloodstream. In a healthy person, with a decrease in the level of sugar, insulin production is suspended, but this limiting mechanism does not work for insulinoma cells.
 Primarily, the central nervous system suffers from hypoglycemia, since glucose is the most important source of energy for brain activity.In conditions of an energy deficit, neuroglycopenia develops, manifested by a wide range of neurological and psychiatric disorders .Against the background of a long lack of carbohydrate in the central nervous system, there are changes in the dystrophic nature( often irreversible).Deficiency of glucose provokes the release of norepinephrine, cortisol, glucagon and STH( somatotropin).These contrinsular hormones in turn determine adrenergic clinical manifestations of pathology.
Primarily, the central nervous system suffers from hypoglycemia, since glucose is the most important source of energy for brain activity.In conditions of an energy deficit, neuroglycopenia develops, manifested by a wide range of neurological and psychiatric disorders .Against the background of a long lack of carbohydrate in the central nervous system, there are changes in the dystrophic nature( often irreversible).Deficiency of glucose provokes the release of norepinephrine, cortisol, glucagon and STH( somatotropin).These contrinsular hormones in turn determine adrenergic clinical manifestations of pathology.
Insulinoma is characterized by alternation of latent phases, hypoglycemic seizures and periods of reactive hyperadrenalineemia .In the period of temporary stagnation( comparative well-being), signs of a hormonally active pancreatic tumor are only an abnormally high appetite( the body tries to fill the lack of energy substrates).On its background, obesity is not ruled out.
Acute hypoglycemic attack is a direct consequence of the failure of the CNS adaptive mechanisms in combination with the inadequacy of counterinsular hormonal factors.
Important: develops a pathological condition on an empty stomach.At the peak of the attack, the blood glucose level drops to critical figures( ≤ 2.5 mmol / l).
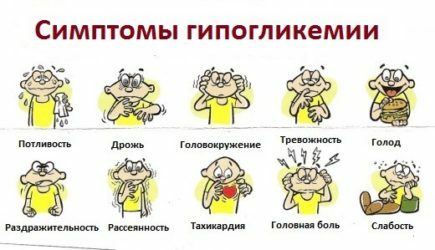
Neuro-glycopenic symptoms:
- intense headache( cephalalgia);
- movement coordination disorder;
- muscle weakness;
- impaired consciousness;
- psychomotor agitation( hyperkinesia, aggression, hallucinations, euphoria).
Characteristic signs of reactive hyperadrenalineemia:
- abundant cold sweat;
- tremor( trembling of limbs);
- acute hunger;
- rapid pulse( tachycardia);
- sensitivity disorders( paresthesia);
- Feeling of fear.
Important: acute hypoglycemia is removed by IV injection of 5% glucose.After normalization of the patient's memory, the information about the seizure is not saved.
Against the backdrop of a sharp drop in glucose levels, myocardial nutrition is disturbed, which can lead to its ischemia, and, as a consequence, a heart attack.With frequent episodes, men may experience sexual impotence.
During the period between attacks, the following are noted:
-
 muscle pain;
muscle pain; - neurological symptoms;
- deterioration of the ability to memorize;
- decreased cognitive abilities;
- visual impairment;
- apathy.
Malignant insulin is characterized by such additional clinical manifestations as pain in the abdominal region, a sharp decrease in body weight( cachexia), paresis and frequent diarrhea.
Diagnosis of insulinoma
Note: is the most commonly insulinoma diagnosed in mature and elderly patients( 40-60 years of age), and in children only in rare cases( no more than 5%).
Because insulinomas are characterized by small dimensions, physical examination is not particularly important.
Functional tests are required for diagnosis.Especially important is the evaluation of blood glucose, insulin, proinsulin and C-peptide.
In patients with insulinoma, the so-called."Hunger test" causes Whipple's triad specific for this tumor pathology:
- is a bright manifestation of neuropsychic symptoms;
- decrease in sugar level to ≤ 2.78 mmol / l;
- relief of clinical manifestations of glucose.
Insulin injection leads to a significant increase in the level of C-peptide.
If "provocative tests" are positive, they resort to hardware diagnostics to clarify the localization, size and nature of the lesion.
From selective methods, selective angiography and echography( ultrasound scanning) are considered the most reliable. Magnetically-resonant tomography of the gland and scintigraphy( visualization with preliminary introduction of radioactive isotopes) are also used.It is often necessary to resort to laparoscopic diagnosis, during which a biopsy is performed.A tissue sample is sent to the laboratory for cytological and histological analysis;It makes it possible to confirm or exclude insulinoma malignancy.
Neurological examination reveals:
- nystagmus( involuntary oscillation of the eyeball);
- asymmetry of tendon reflexes;
- vertical paresis of the eye;
- attenuation of abdominal reflexes.
Nonspecific and a variety of insulinoma symptoms require differential diagnosis with neurasthenia, CNS tumors, epilepsy, acute psychosis, VSD, galactosemia, medical hypoglycemia, pituitary insufficiency and malignant adrenal tumors.
Insulin treatment methods and prognosis
Conservative methods of treating insulinoma are ineffective.When the diagnosis is verified, surgery is usually performed.
Possible types of operations:
- enucleation of the tumor( the most gentle method);
- resection of the gland;
- total pancreatotomy( complete removal of the affected organ);
- pancreatoduodenal resection.
The choice of technique depends on the nature of the tumor( benign or malignant), its location and size, as well as the dynamics of the pathological process.
The effectiveness of the operation is determined directly during the intervention by a dynamic assessment of blood glucose.
Possible postoperative complications include:
- Inflammation of the pancreas;
- necrotic organ changes;
- fistula;
- abscesses of different localization;
- Inflammation of the peritoneum( peritonitis).
After the operation, more than 5% of patients die.
If insulinoma is found to be inoperable during the examination, resort to medical therapy, the purpose of which is the prevention and elimination of hypoglycemia. According to the testimony, the patient is prescribed hormonal drugs - glucocorticoids, adrenaline or norepinephrine.
If a malignant character of the tumor is detected, chemotherapy is required.
Basic chemotherapeutic agents shown in insulinoma:
- 5-fluorouracil;
- Streptozotocin;
- Doxorubicin.
Achieving full clinical recovery is possible with early diagnosis and timely operation.Positive results can be achieved in almost 80% of patients. Approximately 3% of cases of insulinoma recur.
After removal of the tumor, encephalopathy and signs of decreased intelligence are most often retained.In many patients, this leads to a loss of professional skills and a change in social status.However, if the operation is done on time, regression of pathological changes from the side of the nervous system is possible.
For malignant tumors, the prognosis is least favorable - the two-year survival rate is not more than 60%.
All patients who have been diagnosed with this tumor should be on a dispensary record with a neurologist and endocrinologist.
Vladimir Plisov, medical reviewer