Gastroscopy: preparation, indications and interpretation of the results

Esophagogastroduodenoscopy( gastroscopy) is a procedure in which a mucous membrane of the esophagus, stomach and duodenum is examined using a special device - an endoscope.The endoscope is nothing more than a thin flexible enough tube with a camera and a backlight on the end.The image itself is displayed on the screen of the monitor, which allows to study in more detail the state of the mucous membrane of the digestive tract.
In the people this procedure is called "swallowing a probe", and the ideas about it are filled with fears and fears.Indeed, this is not the most pleasant manipulation, but if all the necessary conditions are met, it can pass quite calmly.In addition, if there are gastroenterological problems, this method will help determine the diagnosis.
Indications for Contraindications Preparation for gastroscopy Evaluation of resultsIndications for
Esophagogastroduodenoscopy( EFGDS) is a highly informative diagnostic method for suspected gastroenterological diseases. The following symptoms may be the cause of the manipulation:
- Abdominal pain;
- Pains in the pit of stomach that occur after eating;
- Heartburn;
- Swallowing disorder;
- Pain when swallowing;
- Nausea;
- Vomiting of food taken on the eve;
- Vomiting of blood;
- Black feces( melena);
- Anemia;
- Severe weight loss;
- Diarrhea.
EFGDS can carry out not only diagnostic, but also medical purpose. Diagnostic indications for the procedure are:
- Clarification of the localization of the pathological process( erosion, ulcers, polyps, neoplasms);
- Detailed visual examination of revealed pathological changes;
- Monitoring the effectiveness of the treatment;
- Differential diagnosis of diseases of the stomach and duodenum;
- Biopsy of affected areas( ulcers, neoplasms).
Carrying out of EGFDS for medical purposes is carried out for the removal of foreign bodies, tumors of small size, stopping bleeding and sclerosing varicose dilated esophageal veins.
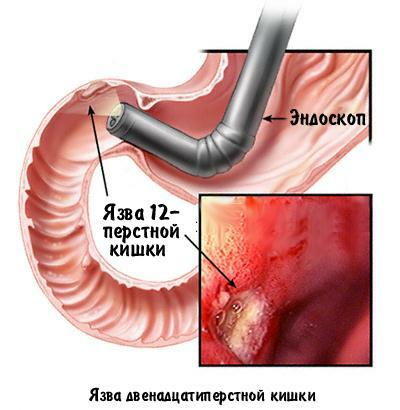
Contraindications
Like any other diagnostic procedure, the gastroscopy has its contraindications.Thus, the manipulation is not carried out with shock conditions, cerebral and coronary circulation disorders, epileptic seizures, exacerbations of bronchial asthma, and also in those cases when the endoscope can not be normally inserted into the stomach cavity( with esophagus burns, cicatricial narrowing of its lumen).
 But if the gastroenterological disease poses a threat to life, even if there are contraindications, conducting an EFGDS is absolutely justified.
But if the gastroenterological disease poses a threat to life, even if there are contraindications, conducting an EFGDS is absolutely justified.
There are also relative contraindications, in the presence of which the doctor decides whether it is expedient to conduct the procedure.Among such contraindications are given to whom, coagulopathy, IHD, aneurysm of the thoracic part of the aorta, hypertensive crisis, acute inflammatory diseases of the pharynx and respiratory organs.
Preparation for gastroscopy
Esophagogastroduodenoscopy is performed in a specially equipped office of a polyclinic or hospital.The patient should come with an empty stomach, it is recommended to refrain from eating and even liquid eight hours before manipulation.That is, if the procedure is scheduled for the morning, you need to try to have the last meal until eight in the evening, and in the morning nothing to eat or drink.A very bad decision is the use of alcohol on the eve.This can increase the gag reflex in gastroscopy.
Some time before the procedure, the patient is given a sedative, often seduksen.Approximately 20-30 minutes the doctor conducts premedication with cholinolytics( solution of atropine sulfate or platyphylline).
 Five minutes before the manipulation begins, the patient is given a local anesthetic.To do this, the back wall of the pharynx, as well as the root of the tongue, is treated with 1-2% lidocaine solution by irrigation.And after that they ask the patient to swallow, so that the anesthetic reaches the esophageal opening.After five minutes, the patient feels numbness in the throat, difficulty swallowing, which means that anesthesia has already worked.
Five minutes before the manipulation begins, the patient is given a local anesthetic.To do this, the back wall of the pharynx, as well as the root of the tongue, is treated with 1-2% lidocaine solution by irrigation.And after that they ask the patient to swallow, so that the anesthetic reaches the esophageal opening.After five minutes, the patient feels numbness in the throat, difficulty swallowing, which means that anesthesia has already worked.
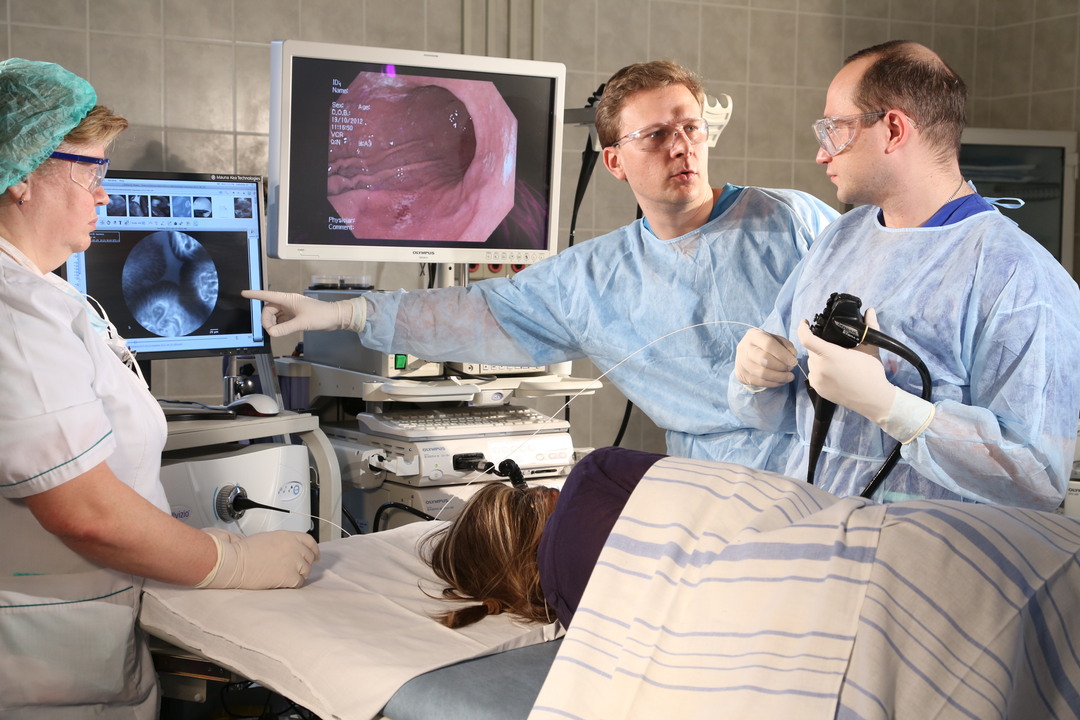
The patient is placed on the prepared table on the left side.The legs are usually brought to the stomach, hands along the trunk.Under the head of a man put an oilcloth.The doctor becomes a face to the patient, gives the mouthpiece and asks to clench his teeth.An endoscope is inserted through the mouthpiece into the oral cavity.The patient is offered to take a breath while inhaling, at which point the doctor neatly moves the endoscope.
As the patient makes swallowing movements, the endoscope moves deeper into the esophagus.Gradually promoting the device, the doctor examines the condition of the mucosa of the esophagus, then the stomach, 12 duodenal ulcer.The duration of the EGFDS is usually ten to fifteen minutes.If necessary during the gastroscopy, therapeutic manipulations can be performed: removal of the polyp, stopping the bleeding, then the procedure will take a little longer.After a detailed study of the mucous membrane of the digestive tract, the doctor neatly pulls out the endoscope.
Gastroscopy can be performed under general anesthesia, so that the patient does not experience discomfort during manipulation.Anesthesia is carried out with the help of modern short-acting drugs.That is, the patient is anesthetized only during manipulation, and after it comes to an end comes to his senses.The procedure under anesthesia is also called "Gastroscopy in a dream."
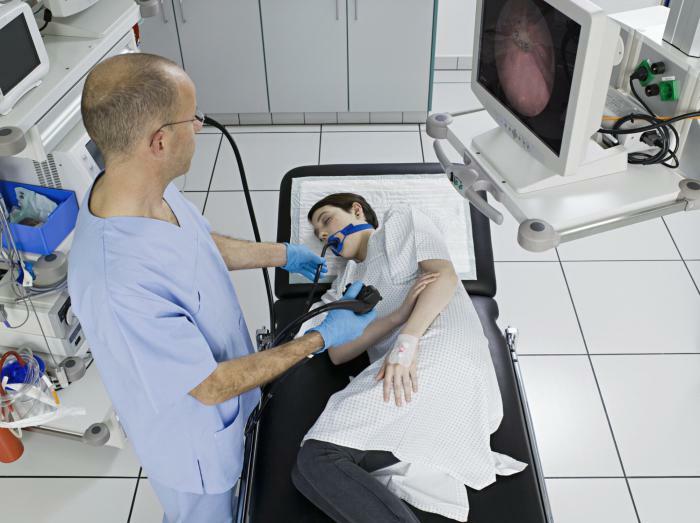
The emotional state of the patient affects the way the sensations are treated.So, it is difficult for experienced and excited individuals to breathe properly, in a measured manner, when the probe is propelled, they constantly choke, and a vomiting reflex may increase.Therefore, it is in the interests of the patient himself to have a good night's sleep and come to rest, calm to the procedure.
Remember: The less resistance a patient is, the easier and faster the gastroscopy is.
Evaluation of results
Normally, the mucous membrane of the stomach is pink.In the anterior part of the stomach the mucous membrane is smooth, shiny, covered with a small amount of mucus, and in the back - folded.The gatekeeper has a conical shape, with a black round hole in the depth, its appearance is constantly changing.When the gatekeeper is opened, the dark, rounded cavity is visualized, when it contracts - its folds become stellate.
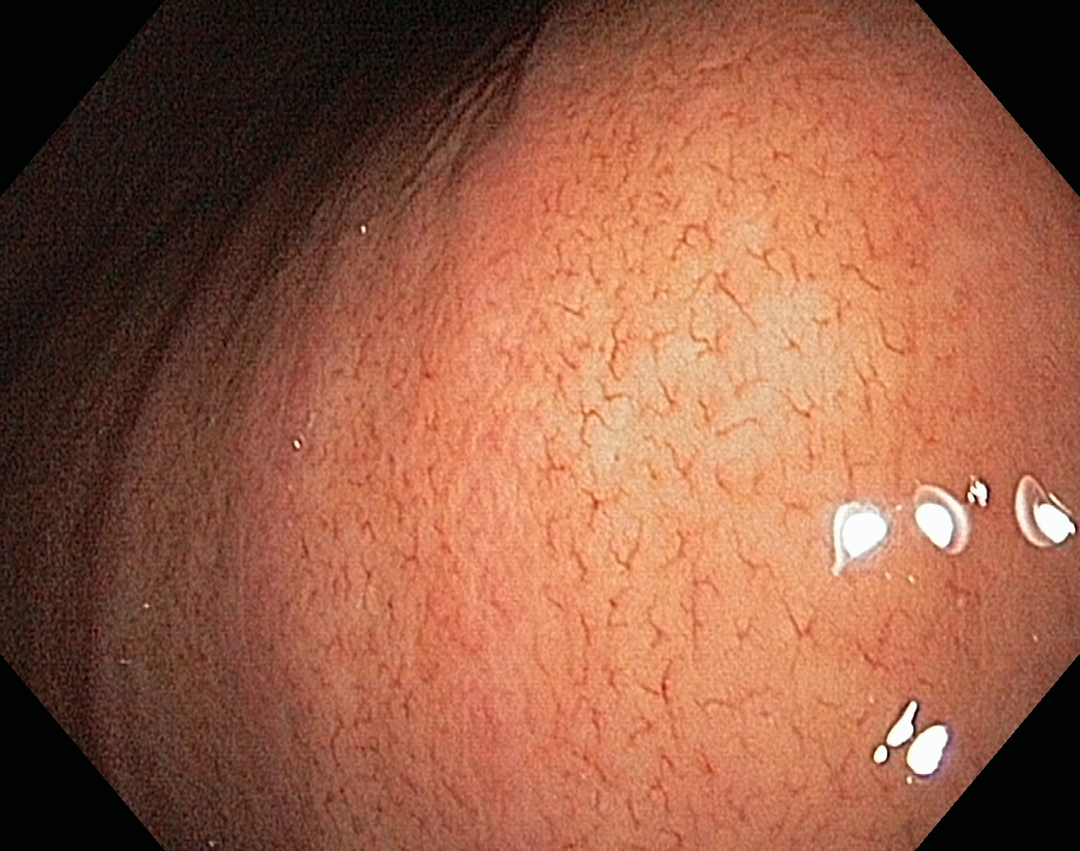
In patients with gastritis, the gastric mucosa is red, swollen with thickened folds.In the submucosal layer, scattered hemorrhages are seen.Another sign of gastritis is the presence of mucus, and it is firmly fixed to the gastric folds.
In case of peptic ulcer during examination of the gastric mucosa, a peptic ulcer with a conical shape is visualized, and around the edges it is surrounded by a roller.The bottom and edges of the ulcer are bright red, sometimes cyanotic.If there was a hemorrhage in the area of the ulcer, its bottom acquires a brown tint.If the ulcer is healed, it becomes a whitish spot.Evidence of malignancy of the ulcer is indicated by thickening, unevenness, nodularity of the edges of the ulcer.
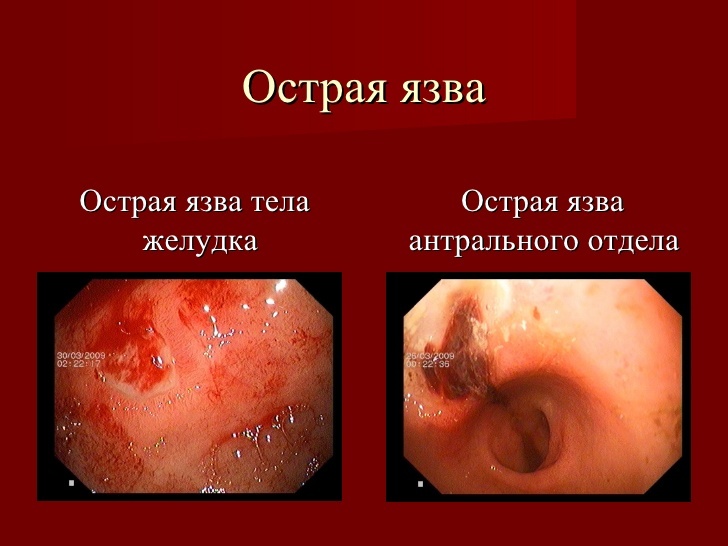
With diffuse infiltrative gastric cancer, the mucous membrane of the organ is smoothed out, has a grayish white color.In polypoid cancer, it is possible to visualize a clearly delineated tumor with a wide base, cylindrical or spherical.Its surface can be smooth or on the contrary bumpy, often with erosion.
Grigorova Valeria, medical reviewer