Symptoms and treatment of diabetic foot, foot care for diabetes
 Diabetes mellitus is a severe chronic disease that is accompanied by various complications.And the most dangerous is the diabetic foot syndrome - it develops in 15% of patients with diagnosed diabetes more than 5 years ago.
Diabetes mellitus is a severe chronic disease that is accompanied by various complications.And the most dangerous is the diabetic foot syndrome - it develops in 15% of patients with diagnosed diabetes more than 5 years ago.
In medicine, there is a clear definition of of the diabetic foot syndrome - these are changes in the nervous system of a pathological nature, as well as violations of arterial and capillary blood circulation, which lead to the formation of necrotic ulcers and gangrene on the feet.
We recommend to read:Under the diabetic foot syndrome, abscesses, osteomyelitis, trophic ulcers, purulent arthritis, tendovaginitis, diabetic osteoarthropathy are meant.
Table of Contents:Causes of Diabetic Foot Syndrome
If a person has diabetes mellitus, this means that his pancreas produces an inadequate amount of the insulin hormone, which ensures the passage of blood glucose to all internal organs.But since insulin is not enough, it means that part of the glucose remains in the blood, which eventually leads to violations of blood flow in the vessels, damage to nerve fibers.Lack of blood circulation( in medicine it is classified as ischemia) provokes long-term healing of wounds, and nerve damage - loss of sensitivity.
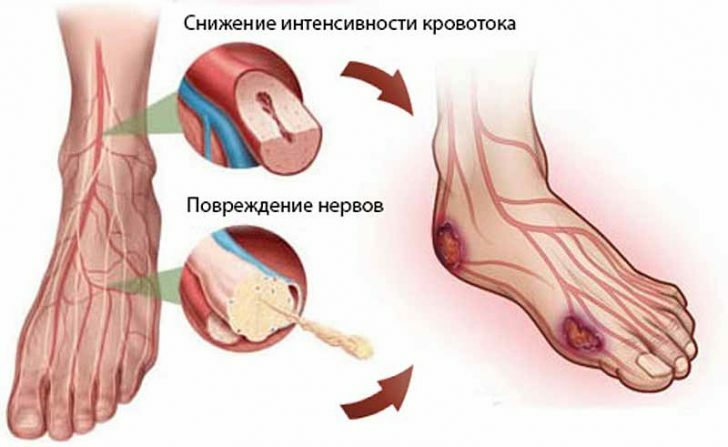
All these disorders lead to the formation of trophic ulcers ( they eventually develop into gangrene) - absolutely any trauma to the skin of the foot( even small cracks) turns into open sores.If a person has on the foot of calluses and keratinized skin areas, then underneath will form hidden ulcers.
Typically, the foot damage occurs in those places where the main physical load is assigned - they knowingly lose some sensitivity and the person simply can not immediately determine the cracks or microrails.And such damages are the "gates" for infection - that's the favorable environment for the development of purulent pathology.
If you combine all the data, you can clearly identify the main causes of the development of diabetic foot syndrome:
- blood flow disturbance in the arteries and capillary vessels;
- decreased sensitivity of the lower limbs;
- deformation of the feet;
- increased dryness of the skin.
Diabetic distal neuropathy( decreased sensitivity)
Nerve damage in diabetes mellitus is due to the constant exposure to them of too high blood glucose levels.But in itself such a pathology can not be the cause of diabetic ulcers - the whole process of their formation proceeds somewhat differently.
First, cracks, abrasions and wounds on the foot do not bother the patient for a long time - he does not take any actions to treat them.The rate of healing of lesions is small, so a purulent process begins to develop.
Secondly, if a person wears tight, uncomfortable or high-heeled shoes, the existing skin damage is simply aggravated, and the newly formed sores begin to expand and "go" deeper.Such uncontrolled trophic ulcers affect both muscle tissue and bone - this leads, ultimately, to gangrene and the need for leg amputation.
Note: According to statistics, leads to wearing tight / uncomfortable shoes in 33% of cases, in 13% - excessive thickening of the skin and in 16% - incorrect handling of the foot with sharp objects.
Blood flow disorder
Arterial blood flow deterioration is always associated with atherosclerotic plaques, and atherosclerosis , proceeding against the background of diabetes mellitus, always passes in severe form and rapidly. Features of atherosclerosis in diabetes:
- under the influence of the disease, arteries of the lower leg( lower legs);
- damaged arteries at once both legs and even in several areas simultaneously;
- atherosclerosis is diagnosed even at an early age in diabetes mellitus.
Violation of blood circulation in the arteries of the legs leads to oxygen deficiency in the foot tissues, which in turn provokes necrotic changes.In addition, the disturbed blood flow helps slow the healing of wounds, and all together and causes the formation of necrotic ulcers on the patient's foot.
Note: atherosclerosis can cause the formation of trophic ulcers in a patient with diabetes mellitus even without any damage to the skin.The skin just stops receiving the right amount of oxygen and its cells die, and if a person has also traumatized this area with dying cells, then the spread of trophic ulcers will be inevitable and rapid.
The most severe consequence of diabetic foot syndrome is leg amputation and the spread of purulent infection throughout the body - sepsis, which almost always leads to the death of the patient.Therefore, diabetics should know exactly the first signs of the development of the syndrome under consideration, methods of combating it and prevention measures.
Symptoms of diabetic foot
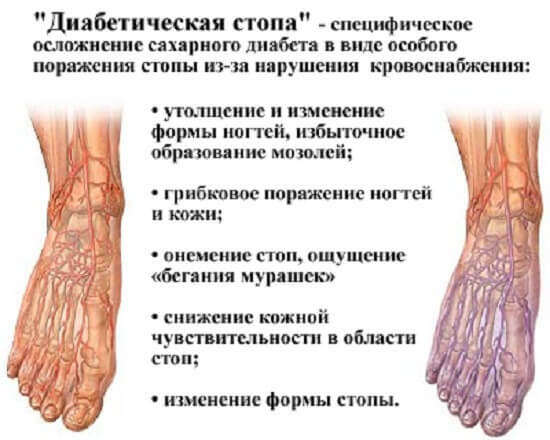
What should alert a patient with diabetes:
- reduced tactile, temperature and pain sensitivity of the feet;
- permanent, long not passing, edema of the lower limbs;
- constant decrease and fever temperature increase - they will be either very hot or excessively cold;
- at walking strong fatigue is felt, legs or foots start to hurt or be ill; be sick literally in 10-50 meters of the passed way;
- regularly present aching pain in the shin - it is present when walking and at rest;
- unaccustomed sensations in the feet 'feet - tingling, burning, chilliness;
- the skin of the legs begins to change color - they can become too pale, cyanotic or red spots may appear;
- a change in the structure of the nail plate and bruises under it - this indicates a fungal lesion that provokes necrosis;
- too long healing of even small wounds and calluses - instead of 2 weeks the process lasts 1-2 months, and after healing there are dark traces on the skin;
- ulcers on the soles of the feet.
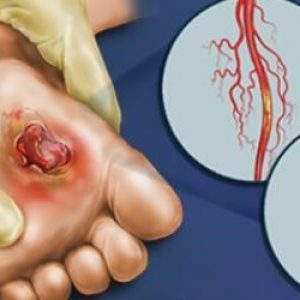 It is necessary to inspect the feet daily, especially carefully monitor the condition of the skin in the interdigital space.If there are any changes, you need to seek advice from a specialist - it's better to let the alarm turn out to be false, than the precious time will be missed and reach the amputation of the lower extremities.
It is necessary to inspect the feet daily, especially carefully monitor the condition of the skin in the interdigital space.If there are any changes, you need to seek advice from a specialist - it's better to let the alarm turn out to be false, than the precious time will be missed and reach the amputation of the lower extremities.
Note: patients with diabetes should visit the doctor at least once a year to inspect and assess the condition of the feet.
In medicine, there are two forms of the diabetic foot syndrome - neuroischemic and neuropathic . With the neuroischemic diabetic foot:
- , the hair begins to fall on the lower leg;
- of the foot becomes cold;
- the skin begins to blush, and the sole acquires a cyanotic shade;
- ulcers are formed on the ankles and heel;
- ulcerous surface does not have exudate, practically dry;
- tenderness in the lesion is clearly pronounced;
- the skin around the trophic ulcer is thin and dry.
There are a number of risk factors for the development of the neuroischemic diabetic foot:
- previously diagnosed ischemic heart disease;
- stroke;
- elderly patient;
- increased amount of cholesterol in the blood;
- smoking.
Distinctive characteristics of the neuropathic form of the disease under consideration:
- the skin color remains within the norm, it can become more pink;
- stops are always excessively warm;
- ulcers are formed in places of excessive physical exertion;
- wound is always wet and almost painless;
- the skin around the trophic ulcer is coarse, horny.
Risk factors for the neuropathic diabetic foot are young age, diagnosed type 1 diabetes mellitus and excessive consumption of alcoholic beverages.
How is diabetic foot syndrome diagnosed
? At the first changes, similar to the symptoms of a progressive diabetic foot, it is necessary to seek professional medical help.The doctor will certainly conduct a series of tests that will not only accurately diagnose, but also assess the patient's condition. As part of the diagnosis of the examined disease, the following tests are performed:
- general and biochemical blood test;
- check of kidney function and general urine analysis;
- ultrasound examination of the heart;
- chest X-ray;
- blood coagulation test;
- sensitivity test for tactile and pain;
- checking the safety of reflexes;
- measurement of pressure in the vessels of the limbs;
- if there is already a trophic ulcer, the doctor examines its contents and sends the biomaterial for examination to the laboratory;
- X-ray of the feet and joints of the lower limbs.
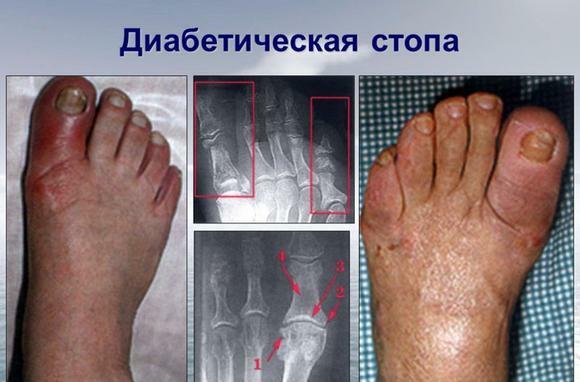
Treatment of diabetic foot
This syndrome is a dangerous complication of diabetes, therefore, it is necessary to conduct treatment.
If the blood flow in the lower limb is not impaired:
- The ulcer is regularly and thoroughly handled;
- provides relief of the limb - the patient is prescribed bed rest or movement with crutches, wheelchair;
- for the suppression of infection, the course of antibiotic therapy;
- compensation for diabetes;
- complete rejection of bad habits;
- treats all having ailments that can hinder the healing of ulcers.
If it is found that the blood flow in the limbs is impaired, the doctor conducts all of the above measures and therapy to restore blood flow.In some cases, surgical intervention may be necessary.
If the patient asked for medical care with the already existing deep trophic ulcers, then first he is treated for necrosis, and if ineffectiveness - amputation.
Treatment of ulcers
After examination, the doctor removes tissue that has already lost its viability - so stops the spread of the infection.Then a mechanical cleaning of the wound from the collected liquid is carried out.It is strictly forbidden to use greengroke, iodine or alcohol when treating trophic ulcers - they further damage the tissues.Wash the wound with a physiological solution or antiseptics.
Unloading of the limb
This point is very important in the treatment of diabetic foot syndrome, because the sensitivity is reduced, and the patient is absolutely calmly resting on his foot even with an extensive trophic ulcer.If the ulcers are located on the lower leg, the doctor will recommend shortening the time in the vertical position, if the wound is on the back surface of the foot, then you should rarely wear street shoes and give preference to soft house slippers.In each specific case, recommendations for unloading the limbs will be individual.
Suppression of infection
As long as the infection "rages" in the leg, no treatment methods will help to get rid of trophic ulcers.Therefore, the appointment of a course of antibacterial drugs is strictly necessary in the neuroischemic form of the syndrome in question, and in the case of a neuropathic form, antibiotics are prescribed in 2/3 of all cases.
Regulation of blood sugar
High blood glucose levels have a pernicious effect on blood vessels and nerves - this does not allow healing of already existing ulcers and provokes the formation of new ones.Only properly selected doses of insulin, the installation of an insulin pump can significantly reduce the burden on the body and reduce the risk of developing a diabetic foot syndrome in general to a minimum.
Treatment of co-morbidities
Diabetes mellitus itself is quite a complex disease, but if some other pathologies "join" it, the patient's condition will deteriorate rapidly, trophic ulcers spread extensively and all this will lead, at best, to amputation of the extremities. The most dangerous "satellites" of diabetes are:
- anemia;
- Renal failure, occurring in chronic form;
- poor nutrition;
- oncological diseases;
- disorders of liver function;
- depression;
- treatment with hormones and cytostatics.
Restoring blood flow
With the neuroischemic form of the diabetic foot syndrome, the vessels are so affected that even a small ulcer can not be healed.In this case, the doctor will necessarily conduct therapy to restore blood flow, as otherwise the patient is threatened with limb amputation.
Usually drugs are not able to cope with the task, so the patient undergoes surgical treatment - bypass and / or intravascular surgery.
Surgical treatment of ulcers
The concept of surgical treatment of the syndrome under consideration includes:
- cleansing and drainage of deep ulcers;
- removal of dead bones - this often happens with osteomyelitis;
- plastic surgery for wound defects;
- limb amputation.
Limb amputation is an extreme measure that is undertaken by physicians only under certain indications.After removal of the gangrenous limb, the patient will need to undergo a long period of rehabilitation and take specific medications for healing stump.
How to take care of your feet
It is very difficult to treat a diabetic foot, but it is quite possible to prevent the development of this complication.Diabetes mellitus refers to chronic diseases, so the patient will simply need to constantly carry out grooming procedures behind his legs - this will become a habit.
The very first thing is to learn how to choose the right shoes, because in most cases this factor plays a big role in the development of the syndrome under consideration.
Criteria for choosing the right footwear:
- is made of genuine leather, soft and without internal rough seams;
- absolutely freely passing on completeness and the size;
- home slippers should be with a closed toe and heel;
- street shoes with wide closed socks;
- heel should be 1-4 cm.
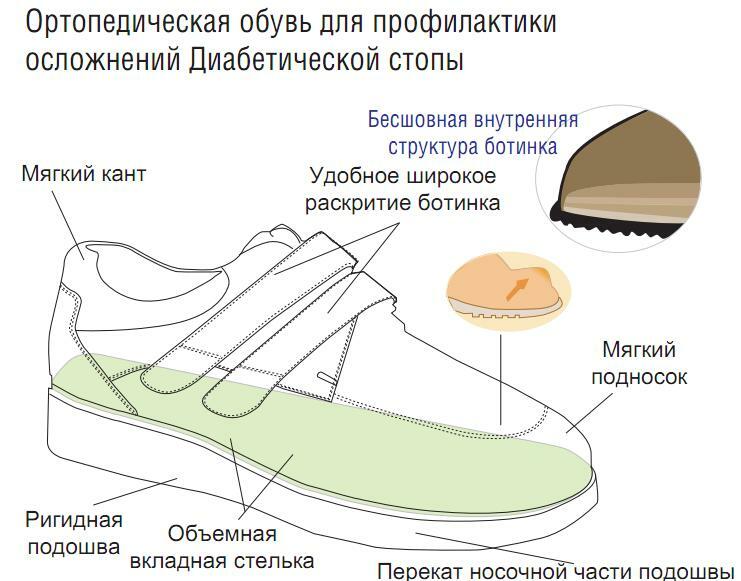
Please note: shoes must be individual, and buy it better after dinner, when the leg is already slightly swollen.
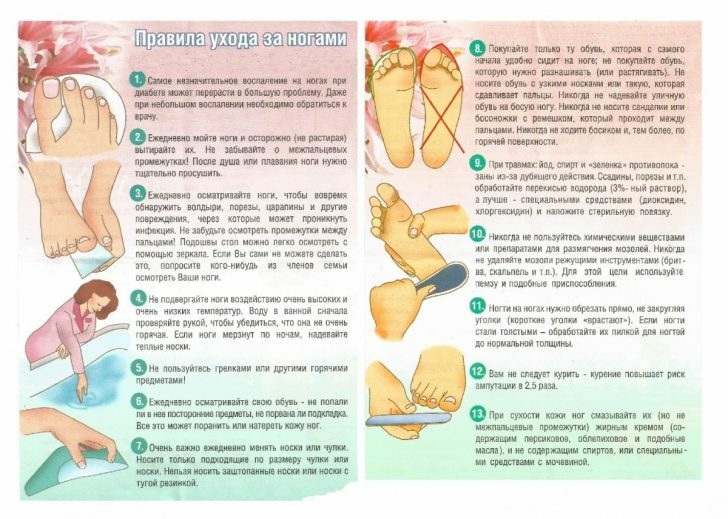
But besides the skill to choose the right shoes, you need to remember a few rules for taking care of your feet:
- Absolutely any abrasions, cuts and injuries of the legs are the reason for contacting a specialist.
- Every day you need to inspect your feet, especially carefully - in hard-to-reach places.Such an approach will help to notice changes in time and start treatment.
- Necessarily every day you need to wash your feet and carefully dry them with a soft towel.
- If there is already a violation of sensitivity, then you need to carefully monitor the temperature of the water in the bath when bathing.Hot baths and hot water bottles are excluded - they can trigger a burn.
- In the winter months, you should never allow hypothermia of the legs.
- Before you put on your shoes, you need to make sure that there is no sand and small pebbles in it.
- You need to change socks and tights every day, it's better to use such things from natural materials.
- It is not necessary to walk barefoot in the house, on the beach and in the forest - because of the decrease in sensitivity, one can not notice injuries.
- You can not treat the wound with green, iodine or alcohol.
- Corns must never be removed with sharp scissors.
- Cut nails very carefully, and if there is a problem with ingrown nails, then solve it with the help of a doctor.
- If excessive dryness of the skin is present, the feet should be treated with baby cream or sea buckthorn oil.But these means can not handle interdigital spaces.
- With diabetes, Alpresan and Balsamed can be used.They eliminate the dryness of the skin, accelerate the healing of wounds, reduce pain.
Just 15 years ago, the diabetic foot syndrome led to the inevitable amputation of the limbs.But now doctors in every way try to keep the patient's legs, and if the patient himself helps in this, the prognosis of this syndrome will be quite successful.Powerful antibacterial therapy, thorough cleansing of trophic ulcers, hygiene compliance - these are the three conditions that allow you to save the patient's legs.
Tsygankova Yana Aleksandrovna, medical reviewer, therapeutist of the highest qualification category