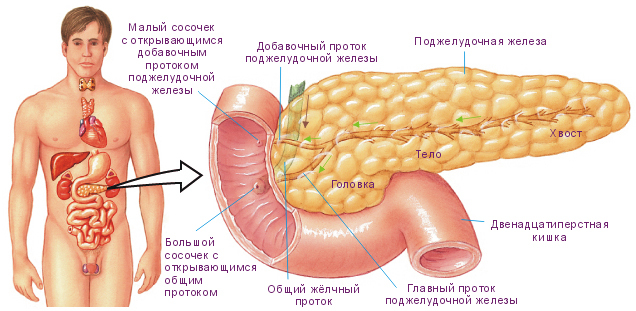
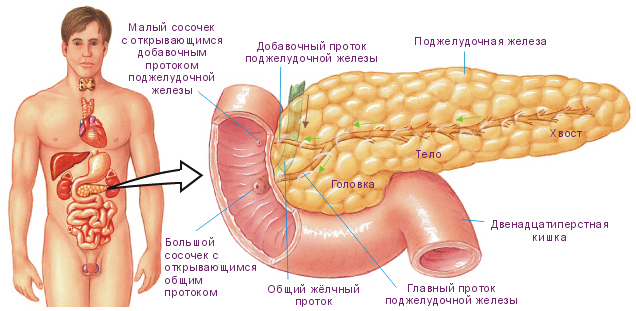
Conduction and consequences of surgery on the pancreas
The need for a surgical operation on the pancreas most often occurs with pancreatitis and cancer.
This is a very serious intervention in the body, the consequences of which can turn the life of the patient upside down.
What are the features of the operation and its forecast - positive and negative consequences? Is it possible to lead a full life after such an operation?
General Information
Contents:
- General Information
- Pancreas Surgery
- Life after Pancreas Surgery
According to some reports, pancreatitis is one of the most common diseases of the digestive system.
In these data there will certainly be a place for overdiagnosis - an ugly phenomenon that is characteristic of Russian medicine, in which diagnostic indicators are "attracted to the ears".However, there is certainly a certain amount of truth in such statistics.
Nutrition does not directly affect the development of the disease, but heavy fatty foods cause gallbladder inflammation and stone formation, and this is one of the factors responsible for pancreatitis.
The prognosis of cholelithiasis indicates that in about 50% of cases it ends with pancreatitis.
Women are more likely than men to develop gallstones and fat metabolism disorders in general, so they are at risk for pancreatitis.
20 - 25% of cases of pancreatitis - the effects of regular alcohol intake. When doctors can not detect the causes of inflammation in the gland, they talk about idiopathic pancreatitis.
This does not mean that there is no reason, but modern diagnostic methods do not always allow you to accurately determine a patient's condition.
Acute pancreatitis can develop as a result of taking various medications: from antibiotics to x-ray contrast preparations.
Diseases, the consequences of which may include the onset of pancreatitis, are viral infections( hepatitis, herpes), bacterial infections, for example, leptospirosis, fungal pathogens, eg candida, parasitic infections.
Acute and chronic pancreatitis are separate pathologies. Acute pancreatitis can have a recurrent form, and on the basis of chronic pancreatitis it can develop acute, and this will not exacerbate the chronic form.
Chronic pancreatitis increases the risk of oncological degeneration of pancreatic tissues.
Among other precancerous diseases are benign pancreas: adenoma and cysts.
Like gastric cancer, a pancreatic tumor is usually diagnosed in later stages, which are characterized by metastasis.
Pain appears in the early stages of the disease, but it is poorly localized, so it is often confused with lumbar pains with radiculitis.
Pancreas surgery
The most dangerous for acute pancreatitis is pancreatic necrosis - the withering away of organ tissues under the action of prematurely activated enzymes that begin to literally digest the gland itself.
In this case, there is an intoxication of the body, which hits the various organs and vital systems, because the poisonous substances quickly spread through the body with blood.
There are three degrees of intoxication: mild, moderate and severe. In the latter case, the operation is more likely to arise.
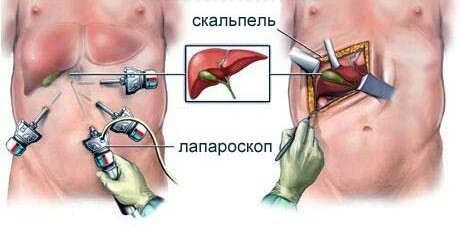
Historically, surgery was the first method of treating inflammatory processes in the pancreas.
However, even at a time when human life was valued little, the lethality of 90 - 100% led to the curtailment of surgical experiments, and the main rate of physicians was made to develop methods of conservative treatment.
The pancreas is considered a fairly "tender" organ, complications can occur even after surgery on neighboring organs.
The main negative effects of surgery on the pancreas are associated with complications: abscesses, infections, massive bleeding and so on.
However, the current level of medical development allows performing quite successful surgical operations on the pancreas.
Under certain conditions, for example, with purulent-necrotic pancreatitis, it is impossible to avoid surgical intervention.
The operation is necessary when pseudocysts are detected - the acquired formation in the pancreas, in contrast to the congenital cyst, as well as in violation of patency of the ducts of the gland or in the fistula.
A separate topic is surgery for oncology of the pancreas. The forecast is conditionally unfavorable.
Physicians managed to reduce the level of postoperative mortality to five percent, however, the five-year survival rate is 8 - 45%.
The survival rate makes pancreatic cancer one of the most dangerous diseases that doctors have ever had to fight.
Video:
However, even if a relapse occurred after surgery for cancer, in most cases the life expectancy is several times higher than without surgery.
In addition, there is such a thing as palliative surgery, when treatment is not aimed at fighting cancer, but to relieve the condition of a dying patient.
Life after operation on the pancreas
Diet( light protein food, refusal of alcohol and carbonated beverages) is of great importance in the treatment of pancreatic diseases:
- diet is one of the strategies for treating organ diseases;
- proper nutrition is necessary for successful rehabilitation after surgery;
- diet is a way to reduce the likelihood and severity of exacerbations in chronic pancreatitis, hence, it serves as a preventive measure to reduce the risk of malignant tissue degeneration;
- is a digestive system, a mechanism all parts of which are in a complex relationship. If failures occur in at least one of its elements, then rational nutrition reduces the likelihood of global disruptions affecting the entire system.
Food processing with pancreatic juice and enzymes contained in it is an important part of digestion.
It is logical that the food after the operation can not be the same. The diet provides for a complete review of the principles of nutrition.
Immediately after surgery, the patient needs an extremely tough diet: a complete lack of food in the early days, then a gradual expansion of the diet.
Approximately 10 days after the operation, you can gradually switch to a diet that will become familiar to the patient.
The diet is based on digestible proteins, wiped food, complete absence of heavy, fatty, fried foods.
Lifetime replacement therapy is needed: enzyme preparations and the use of insulin, without which nutrition is impossible at all.
Several years ago in the United States, the publication of a doctor from California, Murray Ken, about what is more important - the quality of life or its duration, was sensational.
Video:
According to him, doctors who are well acquainted with the possibilities of modern medicine, often refuse from cardinal methods of treatment of fatal ailments, in order to spend the last years, months or days of life among close people, not in the hospital, in the throes of treatment.
No diet, the most healthy diet and modern drugs are not able to provide a high quality of life after removal of the pancreas.
This is the reason why a diet should be a habitual way of life of a healthy person who would like to live long and as fully as possible.