Spermogram: preparation, interpretation, indicators and deviations
Spermogram is a visual, microscopic and physico-chemical study of the ejaculate of men of reproductive age.It allows you to objectively assess the quality and quantity of seminal fluid and its constituent components.The results allow us to conclude not only about the ability to fertilize, but also gives a complete picture of a man's sexual health.
Table of contents: Indications for spermogram Limitations and contraindications Preparation for examination and procedure Normal sperm parametersFor spermogram, the following parameters are evaluated:
- morphological characteristics;
- number and motility of spermatozoa;
- degree of viscosity;
- presence, number and type of leukocytes;
- liquefaction time;
- presence and appearance of imperfect cells;
- color and volume of sperm;
- PH level.
If necessary, an analysis of biochemistry is carried out.
Spermogram is a deep complex study in which possible pathologies of the reproductive system, inflammatory processes and infectious diseases can be identified.
Important! The procedure for taking the analysis is absolutely safe.But it is this study that will help to detect the disease at the initial stage.In time, the treatment started is a guarantee of full recovery.
Indications for spermogram
The study is assigned in such cases:
- in the absence of conception with regular sexual activity throughout the year;
- examination of a man in the planning of pregnancy;
- for diseases leading to infertility( inflammation of the testicles, genital tract injury, varicocele, hormonal disorders);
- for examination and preventive examination;
- as part of an artificial insemination or IVF program;
- treatment control.
Limitations and contraindications
No investigation:
- after stress or heavy physical labor;
- if over the past two months a man has had a fever of 38-39 degrees;
- after prostate massage;
- after taking antibiotics for the past three months;
- with urethritis, orchitis, cystitis and prostatitis;
- immediately after sexual intercourse;
- with exacerbation of chronic pathologies;
- after bath and hot tub;
- in ARI;
- after taking medication or alcohol
Preparing for research and conducting the procedure
Only if certain training conditions are met can you get the most accurate results.
Before passing the test, the following recommendations should be adhered to:
- abstinence from two days to a week.This includes masturbation.During this time the body will develop enough sperm to get the most accurate indicators;
- , when symptoms of a viral illness or cold appear, transfer the analysis;
- at least for a month to refuse from smoking, drinking alcohol, drugs and drugs;
- to avoid mental and physical exertion;
- refuse to visit the sauna or bath.
The sperm for analysis is obtained by masturbation.To collect the material, use a special medical condom or sterile container .In cases where it is impossible to get sperm physiologically, it is done with the help of tools.
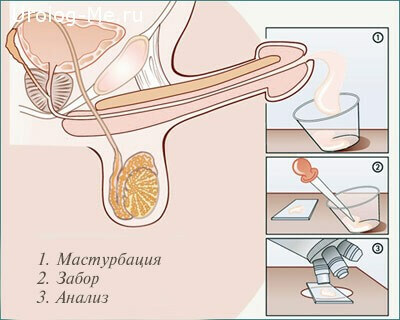
Important! If the material is collected at home, it is delivered to the laboratory no later than one hour after collection.In this case, it should be in an environment close to body temperature.
Normal sperm count
Spermiogram types are distinguished depending on the volume of the study:
- Basic.Carried out according to WHO standards, including all key indicators.
- MAR-test.Determines the presence of antisperm antibodies of different classes that destroy spermatozoa.
- Morphological analysis, or spermogram according to Kruger.
Extended spermogram - all three species together.Assign, if during the baseline study, any deviations were detected.
In some cases, a biochemical analysis of sperm is also prescribed.
Phase contrast microscopy and special dyes - hematoxylin is used to evaluate the function and structure of spermatozoa.
WHO criteria
Indicators of the standard are defined by WHO and include:
- volume of ejaculate more than 2 ml;
- immediately after obtaining sperm viscous;
- after a maximum of half an hour, liquefaction occurs;
- viscosity is not more than 2 cm;
- liquid has a white-gray color;
- specific odor;
- pH indicator 7.2 - 8.0;
- semen is turbid, but there is no slime in it.
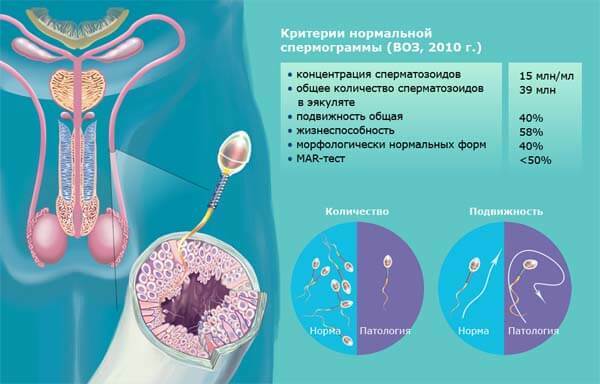
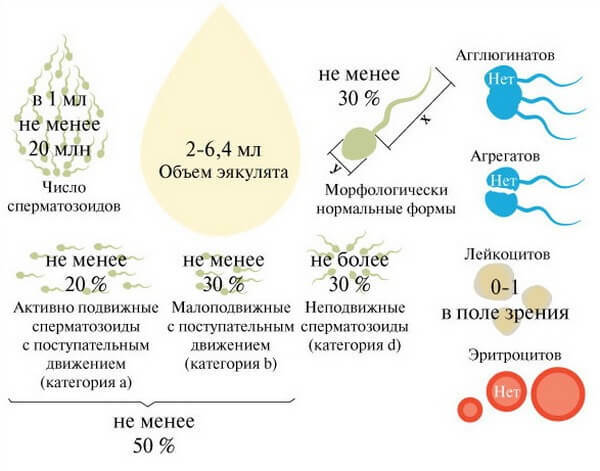
Microscopic indices of the standard
In a microscopic examination, the following parameters are determined:
- in 1 ml of sperm should be kept from 20 ml of spermatozoa;
- mobile should be at least 25%;
- should not be observed gluing and large clusters;
- fixed sperm cells should be less than half;
- of leukocytes - no more than 1 million;
- more than 50% of all cells should be normal sperm;
- more than 30% must be spermatozoa with a normal head structure;
- in ejaculate should not be more than 2-4% of cells of spermatogenesis.
Decoding of the spermogram
The results of the study are evaluated by a specialist, taking into account other clinical data. However, each patient has the right to independently compare indicators with the recommended WHO standard.
-
 The optimal abstinence period is 2-7 days.Ideally, 4 days.When re-submitting the material, the same abstinence period is recommended, as well as before the first procedure.
The optimal abstinence period is 2-7 days.Ideally, 4 days.When re-submitting the material, the same abstinence period is recommended, as well as before the first procedure. - The normal volume of semen is from 2 to 5 ml.
- Normally, the color of the ejaculate should be white-gray.
- The acidity index should exceed 7.2.
- The ejaculate should normally liquefy for an hour.
- For normal viscosity, the length of the filament, when separated from the pipette, should not exceed 2 cm.
- 1 ml of ejaculate should contain more than 20 million spermatozoa.
- The total number of spermatozoa should be 40 million
- The number of structurally normal spermatozoa should be between 40 and 60% of all cells.
- The ejaculate should contain at least 50% of live spermatozoa.
- Agglutination in spermogram should be absent.
- The ejaculate should contain no more than 1 million leukocytes.
- Red blood cells should not be detected.
- Slight amounts of mucus may be present.
Attention! There is no single indicator that would fully confirm absolute infertility, or, conversely, the perfect health of a man.The analysis of indicators can be carried out only by a qualified specialist, considering many other factors.
Possible violations and causes
After the analysis, there may be deviations in the composition of the sperm, as well as changes in its appearance, color and odor.
Violations may indicate the presence of certain problems in the body of a man:
- Oligospermia is when the volume of ejaculate is less than 2 ml.This disease can be caused by insufficient activity of the accessory genital glands, prostate, retrograde ejaculation, decreased passability of the genital tract, a short period of abstinence and insufficient development of sexual characteristics.
- A yellowish shade of semen can be a sign of jaundice.
-
 Decrease or increase in acidity is a symptom of inflammation of the seminal vesicles or prostate.
Decrease or increase in acidity is a symptom of inflammation of the seminal vesicles or prostate. - Viscous ejaculate obstructs the movement of spermatozoa and delays them into the vagina, which drastically reduces the likelihood of fertilization.The causes of slow liquefaction - the lack of enzymes or inflammation of the adnexal sex glands.
- Polyzoospermia - an increase in the number of spermatozoa over 120 million. The cause of the deviation may be endocrine disorders, the effects of radiation and toxins, immune pathology, impaired circulation of the genital organs, inflammation.
- Asthenozoospermia is a severe limitation of motility of spermatozoa.The reasons are the same as in the previous paragraph.
- Necrospermia - the presence in the sperm of dead spermatozoa.It occurs due to infectious diseases, stress, or under the influence of toxins.
- Elevated white blood cells indicate inflammatory processes in the genitals( urethritis, prostatitis, vesiculitis, orchitis, etc.).
- Oligozoospermia - a sharp decrease in the number of spermatozoa in the ejaculate.
- Teratospermia is a low number of spermatozoa with a normal structure.
Reasons for reducing the number of spermatozoa
The main reasons for reducing the number of spermatozoa in the ejaculate:
- diseases of the genitourinary system( cryptorchidism, varicocele, genital tract injury, prostatitis, orchitis);
- prolonged exposure to high temperatures;
- endocrine disorders;
- fever;
- genetic disorders;
- action of toxins.
Reasons for decreased sperm motility
Main factors of low sperm motility:
- antibiotic treatment;
- wearing tight underwear;
- ionizing radiation and electromagnetic waves;
- alcoholism and smoking;
- sedentary work;
- vitamin deficiency;
- frequent use of lubricants;
- stress.
Methods for improving spermogram
The implementation of certain recommendations can significantly improve the quality of spermogram.
-
 Avoid overheating.
Avoid overheating. - Take medications prescribed by a doctor to improve the spermogram.
- To exclude smoking, alcohol and medication.
- Timely treatment of endocrine and urological diseases.
- Observe the mode of the day.
- Adhere to the principles of healthy eating.
- Do exercise, which includes exercises for the muscles of the pelvic floor and abdominals.
- Provide a regular sex life.
To improve the quality of the ejaculate, the doctor can prescribe biological supplements that contain vitamins and amino acids, including carnitine.Additives are actively used in the preparation for IVF and for the treatment of severe oligoasthenozoospermia.
Spermogram is a necessary study to establish an accurate diagnosis and the cause of the disease.
Radevich Igor Tadeushevich, a sexually andrologist of the 1st category