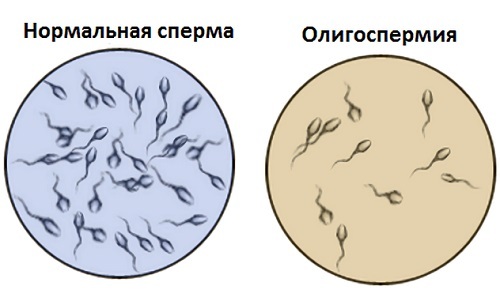
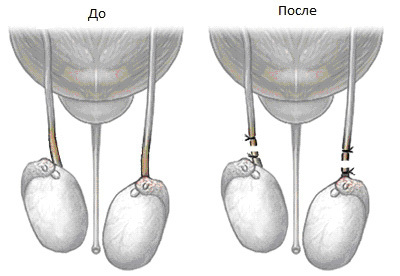
Chronic prostatitis: symptoms, causes, methods of diagnosis and treatment, prognosis Urology

Chronic prostatitis is a serious problem.Even modern urology is not able to answer many questions about this pathology.Experts believe that chronic prostatitis is a disease that is a consequence of a whole range of health problems, which include tissue damage, as well as violations of the functions of not only the urinary tract and prostate gland, but also other organs.
Pathology is diagnosed mainly in men of reproductive age.In elderly men, chronic prostatitis is often accompanied by benign neoplasms of the prostate.
Table of contents: Classification of the disease Symptoms of chronic prostatitis Causes of chronic prostatitis Diagnosis of pathologyClassification of the disease
The classification of prostatitis was developed by scientists of the National Institutes of Health in 1995:
-
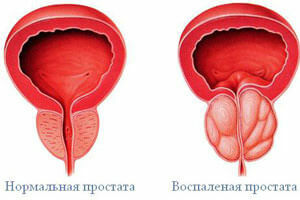 type 1 - acute bacterial prostatitis.It is diagnosed in 5% of cases of inflammation of the prostate gland.
type 1 - acute bacterial prostatitis.It is diagnosed in 5% of cases of inflammation of the prostate gland. - type 2 - bacterial chronic prostatitis.
- 3 type - abacterial prostatitis of chronic course.This pathology has another name - chronic pelvic pain syndrome.
- 3A type - an inflammatory form of chronic prostatitis.Diagnosed in 60% of cases of chronic prostatitis.
- 3B type - non-inflammatory form of chronic prostatitis.Diagnose in 30% of cases.Type
- type - asymptomatic prostatitis.
There is also a classification of chronic prostatitis, compiled in 1990 by Tiktinsky O.L.
Symptoms of chronic prostatitis
Feeling of discomfort and pain in the area of small, which last more than 3 months - the main symptoms of chronic prostatitis.
In addition, there are disorders of urination and impaired erectile function:
- pain occurs in the perineum, can radiate into the anus, inguinal zone, inner thigh, sacrum, loins and scrotum.Pain on the one hand, giving in the testicle is often not a symptom of chronic prostatitis;
- an erection does not occur, despite the available adequate conditions, however, complete impotence is not observed;
- at early stages of the development of the disease, premature ejaculation is observed;
- urination, urinary incontinence, a sensation of pain and burning sensation in the process of emptying the bladder becomes more frequent.
The clinical picture may differ depending on the type of chronic prostatitis.
Infectious form :
- frequent urination at night;
- pain in the thighs, perineum, glans penis and rectum, aggravated by movement;
- painful urination;
- weak urine stream.
Specific infectious:
- mucosal discharge from the urethra;
- the above symptoms.
Non-infectious prostatitis:
- Acute pain in the perineum;
- soreness in the thigh and glans penis;
- pain is exacerbated by the forced interruption of sexual intercourse or the continued absence of an intimate life.
Important! The disease proceeds undulating.Symptoms may then weaken, then increase, but their presence clearly indicates the presence of an inflammatory process.
Symptoms may vary depending on the stage of development of the pathology.
The following stages of pathology development are distinguished:
-
 Exudative. The patient experiences pain in the pubic, groin and scrotum.There is frequent urination and a feeling of discomfort after the end of sexual intercourse.An erection can cause pain.
Exudative. The patient experiences pain in the pubic, groin and scrotum.There is frequent urination and a feeling of discomfort after the end of sexual intercourse.An erection can cause pain. - Alternative. The pain intensifies, localizes in the groin, the pubic part and gives into the sacrum.Urination is rapid, but occurs without difficulty.The erection does not suffer.
- Proliferative. During an exacerbation, urination becomes more frequent.The urine stream becomes weak.
- Scar. There is sclerosis of the prostate tissue.There is a feeling of heaviness in the sacrum and pubic region.Urination is becoming more frequent.The erection becomes weak.Ejaculation may be absent completely.
Symptoms may vary depending on the course of the disease, but in any case they will gradually increase.
Causes of chronic prostatitis
Factors that lead to chronic prostatitis are many.The disease occurs under the influence of infectious agents.The patient has hormonal, neurovegetative, immunological and hemodynamic disorders.Affect biochemical factors, urine reflux into the prostate lobe and disruption of the functioning of growth factors, which are responsible for the proliferation of living cells.
Causes that influence the formation of pathology:
- infections of the genitourinary system;
- physical inactivity;
- irregular sexual activity;
- Continuous catheterization of the bladder;
- regular supercooling.
The development of bacterial disease is facilitated by intraprostatic urine reflux.
Chronic abacterial prostatitis develops against the background of neurogenic disorders of the pelvic floor muscles, as well as elements responsible for the functioning of the wall of the bladder, prostate and urethra.
The formation of myofascial trigger points, which are located next to the organs of the genitourinary system and the prostate gland, can provoke pelvic pain syndrome.Points that are the result of some diseases, surgical interventions and injuries, can provoke pain in the area of the pubis, perineum and adjacent zones.
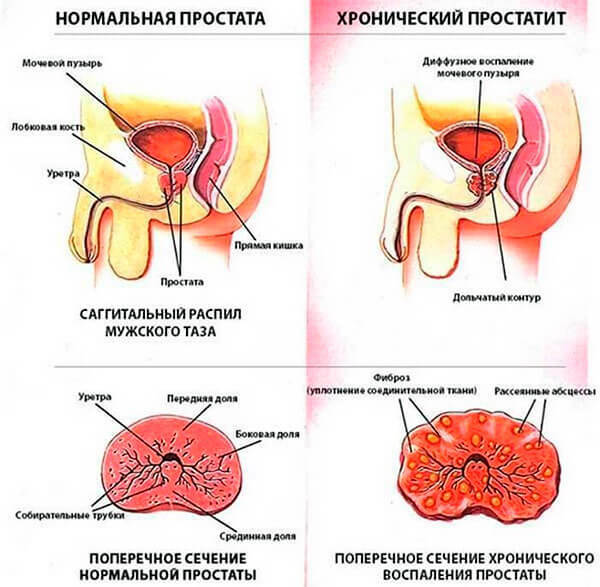
Diagnosis of pathology
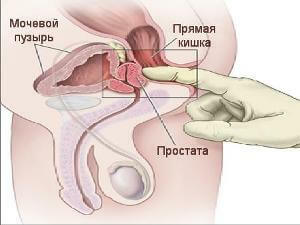 The presence of a complex of symptoms makes it possible to diagnose chronic prostatitis without much difficulty.However, in some cases, the pathology can be asymptomatic.In this case, in addition to the standard examination and questioning of the patient, additional research methods are required. A neurological examination and study of the immunological status of the patient is mandatory.
The presence of a complex of symptoms makes it possible to diagnose chronic prostatitis without much difficulty.However, in some cases, the pathology can be asymptomatic.In this case, in addition to the standard examination and questioning of the patient, additional research methods are required. A neurological examination and study of the immunological status of the patient is mandatory.
Important! Special questionnaires and questionnaires allow you to more accurately determine the subjective feelings of the patient and get a complete picture of the state of health, the intensity of pain, violations of ejaculation, erection and urination.
Laboratory diagnostics
Laboratory diagnostics allows to distinguish bacterial and abacterial form of pathology, as well as to determine the type of pathogen and to provide the most accurate diagnosis. Chronic inflammation of the prostate is confirmed when the fourth urine sample or prostate secretion contains more than 10 leukocytes in the PP, or bacterial associations. When the number of leukocytes is increased, but the bacteria are not sown, the material is examined for chlamydia or other STD pathogens.
- The discharge from the urethra is sent to the laboratory to detect viral, fungal and bacterial flora, leukocytes and mucus in it.
- Scraping from the urethra is examined by PCR.This allows us to identify pathological agents that are sexually transmitted.
- Perform a microscopic examination of the secretion of the prostate for counting the number of macrophages, leukocytes, amyloid bodies and Trusso-Lallemand.Assign immunological examination and bacteriological study.The level of nonspecific antibodies is determined.
- Blood sampling is performed ten days after a digital rectal examination to determine the concentration of PSA in it.At a rate above 4.0 ng / ml, the patient undergoes prostate biopsy to rule out oncology.
Diagnosis is made on the basis of the research results.
Instrumental diagnostics
 To clarify the stage and form of the disease, transrectal ultrasound of the gland will help.Ultrasound can eliminate other diagnoses, monitor the effectiveness of the treatment, and determine the size of the prostate, its echostructure, uniformity and density of seminal vesicles.Identify infravesical obstruction and neurogenic disorders, which often accompany pathology, will allow urodynamic studies and myography of the pelvic floor muscles.
To clarify the stage and form of the disease, transrectal ultrasound of the gland will help.Ultrasound can eliminate other diagnoses, monitor the effectiveness of the treatment, and determine the size of the prostate, its echostructure, uniformity and density of seminal vesicles.Identify infravesical obstruction and neurogenic disorders, which often accompany pathology, will allow urodynamic studies and myography of the pelvic floor muscles.
Tomography and MRI are used to establish a differential diagnosis, in particular, with prostate cancer.These methods will reveal violations in the pelvic organs and the spinal column.
Differential diagnostics
Differential diagnostics are of great importance, since there is a risk that the patient has a more serious disease.
Differential diagnosis is established with such diseases:
- pseudodissinergia, functional disorder of the detrusor-sphincter system, dysfunction of the bladder of neurogenic origin, complex regional pain syndrome;
- stricture of the bladder, hypertrophic changes in the neck of the bladder, prostate adenoma;
- osteitis of the lonnogo articulation, cystitis;
- pathology of the rectum.
If a symptom occurs, it is necessary to examine the prostate gland in a urologist or andrologist .Pass the ultrasound.If necessary, a biopsy of the prostate gland is prescribed.
Methods of treatment of pathology
The treatment of chronic prostatitis is performed by a urologist or andrologist .Therapy is carried out in a complex manner.Correction is subject to the lifestyle of the patient, the features of thinking and his habits.It is important to move more, minimize alcohol intake, get rid of nicotine addiction, eat right and normalize the sexual life.However, it will not work without a course of basic therapy.Taking medications is the main condition for a full recovery.
Indications for admission
The most common treatment is outpatient.But in cases when the disease is not amenable to correction and has a tendency to relapse, the patient is referred to a hospital where the treatment is more effective.
Medical method of treatment
This method is aimed at eliminating the existing infection, normalizing blood circulation, improving the drainage of lobules of the prostate, correcting the hormonal background and immune status.Therefore, doctors prescribe antibiotics, vasodilators, immunomodulators, anticholinergic and anti-inflammatory drugs.
Modern urology uses for the treatment of pathology the following drugs:
- Finasteride;
- Cytokine inhibitors;
- Terazosin;
- Allopurinol;
- Citrate;
- Cyclosporine.
If pathology is of a bacterial nature, antibiotics are strongly recommended. Assay is based on the results of bacterial culture of the secretion of the prostate. This will make it possible to isolate the pathogen and then determine its sensitivity to a particular drug.With a well-designed scheme, the effectiveness of treatment reaches more than 90%.
In the abacterial form, a short-term course of antibiotics is prescribed.It is continued only if the scheme gives a positive result.The effectiveness of therapy is approximately 40%
In chronic pelvic pain, the duration of the course of antibiotics is no more than a month.With positive dynamics, treatment is continued for another month.If the effect is absent, the drug is replaced with another, which may prove to be more effective.
Antibacterial agents from the group of fluoroquinolones are the main drugs for the treatment of pathology. They have high bioavailability, are active against most Gram-negative bacteria, ureaplasma and chlamydia, accumulate in the tissues of the prostate gland.
When treatment with fluoroquinolones is not effective, penicillin preparations may be prescribed.
Antibacterial drugs are used for preventive purposes.
After treatment with antibiotics prescribe therapy with the use of a-adrenoblockers. Such a treatment strategy is effective for patients who have obstructive and irrational symptoms.
If urinary disorders and pain do not go away, tricyclic antidepressants may be prescribed that have an analgesic effect.
With severe urination disorders, urodynamic examination is performed before the start of therapy and act on the basis of the results obtained.
Non-pharmacological therapy
Non-pharmacological methods of therapy make it possible to increase the concentration of antibacterial drugs in the tissues of the gland, but it is not recommended to exceed the dose.
For this purpose, the following methods are used:
- Electrophoresis;
- Laser therapy;
- Phonophoresis;
- Microwave hyperthermia( applied transrectally).
When applying the latter method, the temperature is selected individually.The temperature set in the range of 39-40 degrees, allows to increase the concentration of the drug in the body, activates the immune system at the cellular level, relieves bacteria, removes congestion.Increasing the range to 40-45 degrees allows achieving a sclerosing and analgesic effect.
Laser and magnetic therapy is used in the complex.The effect is similar to the effects of the above methods, but in this case there is also a biostimulating effect on the organ.
Transrectal massage is performed only in the absence of contraindications.
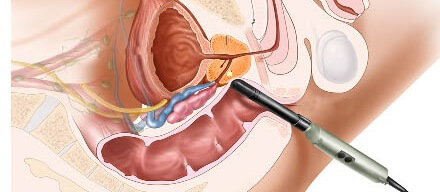
Surgical method
Chronic prostatitis basically does not require surgical intervention.The exception is complications that pose a threat to the health and life of the patient.Modern surgical treatment allows the use of endoscopic surgery.With it, there is minimal invasive intervention.Rehabilitation is faster, and the body causes minimal damage.
Surgical method is prescribed with:
- of prostate sclerosis;
- adenoma of the prostate;
- sclerosis of the seminal tubercle;
- calcinate in the prostate gland.
Important! Surgical intervention is contraindicated in the acute stage.Surgical treatment is prescribed by the surgeon based on the results of the study and the general clinical picture.
Prognosis for chronic prostatitis
Doctors with caution predict the outcome of the disease.To achieve full recovery is obtained in rare cases.Basically, chronic prostatitis passes into the stage of long-term remission.Symptoms disappear, urine and blood levels return to normal.To prevent chronic prostatitis, and did not cause complications, it is necessary to follow all the recommendations of a specialist.
Radevich Igor Tadeushevich, doctor of sexopathologist-andrologist of the 1st category